|
Where mission
and heart meet Behavioral Health. |
|
Can’t access the links? Add “lnks.gd” to the allowlist of your content blocking software. |
|
|
As April comes to a close, we are highlighting timely insights and practical resources that support children, youth, young adults, and families across Washington. This issue reflects the shared work happening across systems to strengthen prevention, increase early connection to care, and support well-being through informed, responsive approaches.
This month’s newsletter includes a focus on Child Abuse Prevention Month and the “Pinwheels of Possibility” campaign, reinforcing the importance of building safe, supportive environments for children and families year-round. We are also elevating emerging and often under-recognized behavioral health needs, including Premenstrual Dysphoric Disorder (PMDD), alongside tools and peer supports that providers and communities can share.
You will also find updates on a significant shift in youth substance use disorder assessment and treatment planning with the release of the ASAM Criteria Fourth Edition for adolescents and transition-age youth, as well as an overview of growing conversations about generative AI, safety, and psychosis. Throughout, the goal is to provide clear information, actionable resources, and relevant learning opportunities to support the work on the ground.
As always, thank you for the leadership and partnership that helps keep youth and families at the center of our systems of care.
|
|
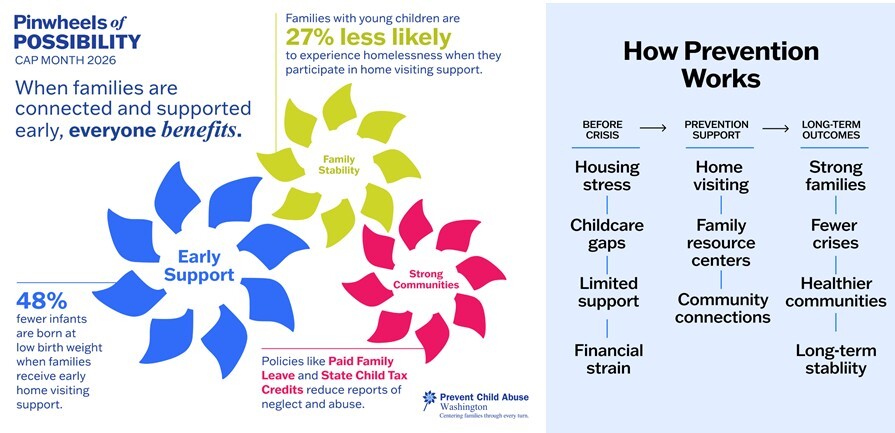
April marked Child Abuse Prevention Month, a time to come together across communities and systems to strengthen families and promote safe, supportive environments for children and youth. This year’s theme, Pinwheels of Possibility, highlighted that when families are connected and supported early, everyone benefits.
Throughout the month, the Department of Children, Youth, and Families (DCYF) and partners across Washington shared prevention messaging and planted pinwheels in communities statewide, including at the State Capitol. These displays served as a powerful reminder of our shared responsibility to support children, youth, and families.
We also recognized National Home Visiting Week (April 20–24), which elevated the impact of early, relationship-based support. Home visiting programs play a role in reducing family stress, strengthening connections, and improving long-term outcomes for children and caregivers.
As April comes to a close, the work continues. Partners are encouraged to keep sharing the Child Abuse Prevention Resource Guide and uplifting prevention-focused messaging within their networks. Increasing awareness, strengthening connections, and investing in early support are key to building strong families and healthy communities year-round.
Together, we can continue creating a culture where children and families thrive, not just in April, but every day.
|
|
|
Our partner, Behavioral Health Catalyst, is hosting a virtual Town Hall to increase awareness of the Washington Thriving Strategic Plan. Newly passed legislation is helping Washington advance efforts to better support behavioral health for young people and families. Governor Ferguson will open the event, followed by a panel, community voices, and a Q&A.
|
|
Explore free resources from the International Association for Premenstrual Disorders (IAPMD), including handouts, informational sheets, research, and peer support. Youth can also join the Young PMDD & PME Support Group: a safe, age-appropriate space to connect, share experiences, and find community.
|
|
For Mental Health Awareness Month, HCA is highlighting Third Places, community spaces outside home, work, or school where people connect and belong. Providers, partners, youth, and families are invited to submit Third Place Spotlights, including location, who it supports, and how it helps well-being.
|
|
|
The American Society of Addiction Medicine (ASAM) Criteria is the most widely used and comprehensive set of guidelines for treatment placement for individuals with substance use disorder. The ASAM Criteria’s standards provide a framework for organizing the addiction treatment system, including the types and intensities of treatment that should be available (e.g. outpatient therapy, residential services). In Washington licensed Behavioral Health Agencies (BHA) are required to use the ASAM Criteria when assessing young people for a substance use disorder.
Since the first publication of the ASAM Criteria in 1991, standards for adolescent care have been interwoven with those for adults. As research on addiction and effective approaches for young people has significantly evolved, ASAM has developed for the first time, a specific and evidenced-based volume for adolescents and transition-age youth. This historic change may be missed by those who don’t actively use this assessment tool in their lives. However, it cannot be overstated that this formal shift to both assess and treat young people in a developmentally, culturally specific, and trauma-informed way is an essential move in the practice of addiction treatment and early intervention. This evolution is also intentional about ensuring mental health is addressed and tended too as needed, for people accessing care for substance use. There is emerging hope that there will now be a uniform and coordinated approach that will be adopted by BHAs across our state to support young people.
The ASAM Criteria, Fourth Edition, Volume 2: Adolescents and Transition-Aged Youth (ATAY) was released this spring. In the 2025 legislative session, SB 5361 was passed delaying the adoption date of the latest edition until January of 2028. While 2028 approaches, work is underway to prepare for this historic implementation, which asks us to build a system that supports our young people with care that is truly tailored and useful for them.
|
|
|
Generative AI applications like ChatGPT are quickly becoming a part of daily life. Yet, many have concerns regarding the safety of chatbots, which seem to reinforce thinking patterns over time—even problematic ones. Research shows how AI may even contribute to new episodes of psychosis and unsafe behaviors in individuals with underlying vulnerability (Hudon & Stip, 2025).
Environmental and social factors, such as isolation, stress, and the convenience of chatbots may influence how and why young people choose to interact with AI. In a recent report from Common Sense Media, young people report use of AI applications for a variety of tasks and seem to have, in general, a more positive perception of this technology than some caregivers.
Behavioral health professionals and advocates are encouraged to be aware of the risks and develop skills in supporting young people and families as they navigate a world increasingly influenced by AI. Digital literacy efforts, safety planning tools, and psychoeducational approaches may be considerations for future development.
Psychiatrist Stephan Taylor, M.D., of Michigan’s early psychosis program advises that if you or someone you know is exploring their mental health with AI chatbots, it is important to speak with a trusted human about what is happening. If you notice or suspect that someone may be experiencing a different reality than others or notice significant changes in behavior, it is important to connect with support.
In Washington State, New Journeys provides specialized treatment for individuals experiencing symptoms, and anyone can make a referral. The earlier a person gets connected to care, the better the outcomes.
|
|
|
Premenstrual Dysphoric Disorder (PMDD) is a serious, yet often overlooked, behavioral health condition affecting an estimated 5.5% of people who menstruate worldwide. For some, symptoms can be severe impacting mood, relationships, and daily functioning. Risk factors include a personal or family history of anxiety, depression, or PMDD. In addition, Premenstrual Exacerbation (PME) can intensify existing mental health conditions during the luteal phase of the menstrual cycle.
Despite being recognized in the DSM-5, awareness of PMDD remains limited across healthcare systems, including within behavioral health settings. This gap in understanding can lead to misdiagnosis, often as bipolar disorder or borderline personality disorder, and delays in effective care. The stakes are high: individuals with premenstrual disorders are at significantly increased risk for suicide.
For youth and young adults, early recognition and appropriate support are critical. Research highlights the impact of PMDD among youth and young adults, including a study on prevalence among school-going girls and additional findings on premenstrual disorders in young adults.
As we continue advancing behavioral health supports from prenatal through age 25, increasing education and dialogue around PMDD is an important step toward more responsive, equitable care for all.
|
|
|
|
|