|
Dear HCMACS Program partners,
This month marks the start of a new direction for our HCMACS newsletter—one that’s less about milestones and more about meaning. Rather than reporting just on status updates, we’ll be sharing stories from the people shaping this transformation every day. You’ll hear about the challenges of today’s systems, the excitement (and sometimes apprehension) around change, and the vision driving us toward a shared electronic health record with shared governance and shared workflows to unify care delivery across multiple state agencies, tribes, and community-based providers who serve safety-net populations. Through these first-hand perspectives, we hope to build a clearer understanding of why this change matters and a stronger shared commitment to making it real.
Thank you to Dr. Morris Seligman, Suzie Ovel, Lisa Gosiaco and the rest of the DSHS HCMACS project and communications teams for creating and letting us share this story.
This story highlights a framework for change that can be used not just at the DSHS project level but across all program agencies and partners. For HCMACS, in the coming days we will work together to understand how care is delivered across all facilities to inform shared workflows and a standard configuration of our foundational system. In the end patients will be safer and care will be coordinated in new and improved ways.
Sincerely,
Carrie Paykoc
HCMACS Executive Program Director
By Dr. Morris Seligman, Deputy Chief Medical Officer, DSHS
This article first appeared in the BHHA September newsletter.
Change is always occurring and can be challenging, especially large, complex change initiatives such as the electronic health record project. There are many facets to this change, impacting staff and services across clinical, technological, business and operational settings. A critical element for changes of this complexity is to identify the necessary culture change. I’ve learned from experience implementing large initiatives, including EHRs, that there are two important aspects to highlight for culture change success: preparing the culture for change; and developing the necessary mindsets to have a successful change.
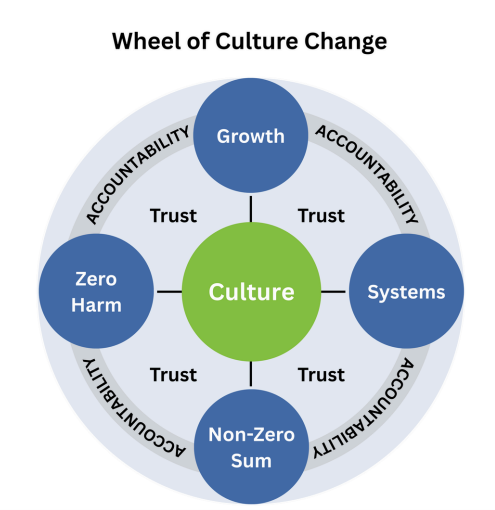
Transitioning from paper-based processes to an electronic EHR platform is a huge culture shift. The wheel shown here identifies the four mindset shifts in thinking necessary to make a culture change. These mindsets are identified as growth, systems, non-zero sum, and zero harm. Let’s break these down.
It begins with having a growth mindset instead of a fixed mindset shift. A growth mindset is the belief that we, and our programs and practices, can continuously improve. It enables practitioners and staff to more easily adapt to new digital workflows and healthcare delivery methods (for example, telehealth) by being resilient and motivated. This is a critical framework for successful EHR implementation by helping healthcare organizations, leaders, and staff navigate the challenges of adopting new technology and processes.
This leads us to systems thinking. This means operating as a single, unified organization to align people, processes, technologies, and data across various facilities, workforces, and care settings.
Systems thinking focuses on analyzing the interconnected components of BHHA to improve patient outcomes, increase equity, enhance quality of care, and reduce costs.
For the EHR project, we need to take the time to understand how care is delivered across BHHA facilities, then implement standardization efforts so that someone working at one facility will see a similar way of caring for a patient with the same diagnosis at another facility.
Making standardization decisions requires people to come to agreement, which is where non-zero sum thinking comes into play. As we standardize processes across our facilities, we want to avoid staff at any facility or program to think of these changes as a win-lose situation, where some staff, facilities or programs walk away as winners and some as losers. Instead, we want everybody to walk away with enough that they feel that they get what they need. This helps us drive toward the goal of zero harm. Zero harm is a safety culture philosophy that aims to eliminate all preventable harm to patients and staff by setting an aspirational goal of zero incidents. A goal of zero harm forces a deeper, more fundamental reevaluation of processes to create safer systems.
I’ve seen in previous change initiatives that when we worked through the process using those four key mindsets, we realized something else occurring: people were holding each other accountable, not only themselves and their teammates, but the organization, the facilities in which they were working, all the way to the leadership level. Because of this it became clear that trust was increasing. Accountability and trust are foundational principles for building strong teams and organizations and driving initiatives for any organization.
The four mindset shifts and the foundational principles are key to changing the culture over time. Ultimately, organizations change because they have the organizational will to change. This requires support from the very top leadership and throughout the facilities. Applying the individual mindsets and the foundational principles, and having the organizational will to change, will help to make our EHR project a success.
|