
|
VHA Office of Community Care
Monthly Provider Updates
 Table of Contents
|

As part of implementing the VA MISSION Act of 2018, VA will offer an urgent care benefit that provides eligible Veterans with greater choice and access to timely, high-quality care. With urgent care Veterans have a new option for care for the treatment of minor injuries and illnesses such as colds such as strep throat, or pink eye.
Eligible Veterans will be able to receive urgent care from an urgent care provider that is part of VA’s and TriWest's contracted network of community providers without prior authorization from VA. VA can pay for an urgent care claim only if:
- The Veteran is eligible for the benefit,
- The urgent care provider is part of VA’s contracted network of community providers, and
- The services are not excluded under the benefit (excluded services include preventive services and dental services).
To learn more, go to TriWest Healthcare Alliance’s (TriWest) website at Training & Support – Proudly Caring for Veterans.
|
|

Many Veterans see providers from the Veteran Health Administration (VA) as well as providers in the community outside of the VA. This can make it difficult for providers to access the records they need to manage a Veteran’s care. By sharing a Veteran’s health information electronically, VA and participating community care providers are better able to coordinate and improve the overall quality of care for our Veterans.
VA Exchange enables bi-directional sharing of Veteran Health Information between the VA and participating community providers. The Information is exchanged over a secure network and includes medical history, allergies, medications, immunizations, problems and more.
For more information on how to participate, please see our VA Exchange Onboarding Flyer and contact VAExchangeInformation@va.gov to get started.
|
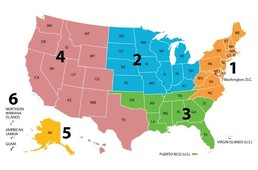
As of May 2, 2019, the Department of Veterans Affairs (VA) is moving forward with implementing Community Care Network (CCN) Region 2 (along with Region 1) in partnership with Optum Public Sector Solutions, Inc (Optum). A kickoff meeting between VA and Optum took place in late May 2019.
In the meantime, VA is continuing with preparation activities. Full deployment dates for Regions 2 are being negotiated between VA and Optum. Both VA and Optum are dedicated to ensuring Veterans are positively affected by this change and that community providers are kept informed of the transition to CCN Regions 2.
|

**PLEASE NOTE CORRECTION IN NUMBER OF DATES TO SUBMIT CLAIMS TO 120 CALENDAR DAYS.**
For all authorizations for care created on or after June 6, 2019, the provider must submit to TriWest Healthcare Alliance Corporation (TriWest) new provider health care claims within 120 calendar days after the date care was furnished.
Questions by community providers about additional contractual procedures details with TriWest can be directed to TriWest Provider Services at ProviderServices@triwest.com or by phone on 855-722-2838, 8 am – 10 pm ET, Monday through Friday.
|

VA continues to provide updates on community care under the VA MISSION Act posted to VA’s official VAntagePoint blog. Updates include fact sheets with more detailed information. To read articles and access the fact sheets, click one of the links below:
Articles:
Fact Sheets:
For more information about the VA MISSION Act and recent information, please see the resources listed below:
|
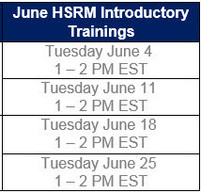

Community providers will be notified when the VAMC(s) you partner with are scheduled to begin using HSRM. In the meantime, the HSRM Team invites you to join us for an overview of HSRM. Every Tuesday from 1 – 2 PM EST, the HSRM Team hosts an introductory training on HSRM’s benefits and functionality. The team encourages you to attend to learn about how HSRM:
- Facilitates Health Information Exchange (HIE) between community providers and VA
- Reduces time community providers spend waiting for calls, faxes, or emails
Registration for one of the weekly introductory trainings can be completed by logging into VHA TRAIN. Please note that a VHA TRAIN account is needed to register. Please follow the link to register.
|

June 20, 2019: VHA Office of Community Care Overview - This webinar provides an overview of Community Care programs and policies, focuses on how to file clean claims, and goes into other topics such as eligibility, referral, top rejection reasons and other provider issues. Register for the webinar.
June 27, 2019: Evidence-based Tobacco Cessation Care in the VA Health Care System: This webinar will provide an overview of evidence-based tobacco use treatment in the VA health care system with a focus on the use of combination nicotine replacement therapy. The goals of behavioral counseling as part of evidence-based treatment will be discussed and there be a review of VA tobacco use treatment resources.
Registration links will be available soon at Provider Education & Training Resources.
Go to the VHA Community Care Provider Education & Training Resources web page for a full listing of upcoming webinars and links to recordings of past webinars.
|
|
|
You have received this message because you are subscribed to the VHA Office of Community Care - Monthly Provider Updates publication, a monthly publication that provides the latest updates that affect VA community providers. Access your Subscriber Preferences to make changes to your subscription or Unsubscribe. Get this as a forward? Sign Up to receive updates from Veterans Health. Having questions or problems? Please visit Subscriber Help for assistance.
|