|
The Oregon Health Authority (OHA) has made the following fee-for-service claim processing updates:
Why is this happening?
OHA covers approved planned community birth services for both CCO and fee-for-service members. Based upon provider feedback, OHA identified procedures that were not processing correctly for coverage and payment. NWRNBS updated its program fees effective 8/1/2022.
What should you do?
For covered community birth services provided on or after 9/1/2021:
For newborn bloodspot screening kits provided on or after 8/1/2022, bill OHA with the following:
- S6320 (2 specimen kit), rate = $175.00
- S6320 with modifier TC (replacement kit for 1 specimen), rate = $100.00
For kits provided before 8/1/2022, please refer to the June 14, 2022 memo from OHA.
With all Medicaid claiming, correct coding and documentation of services provided must be on file to justify the claim. Please refer to Oregon Administrative Rules and the OHP billing page for guidance.
Questions?
Please contact the Provider Services Unit at dmap.providerservices@dhsoha.state.or.us or call
800-336-6016. We are available Monday through Friday between 8 a.m. and 5 p.m. (including lunch hours).
Thank you for your continued support of the Oregon Health Plan and the services you provide to our members.
|
CCO Submitted Address Changes
|
|
Tasks
|
Status
|
Estimated Completion Date
|
|
Submit and receive approval for verification waiver
|
Completed
|
8/1/22
|
|
Create data requirements for secure method for delivery
|
Completed
|
7/15/22
|
|
Create and select secure delivery method for updates coming from CCO to State
|
In Progress
|
8/15/22
|
|
Evaluate and establish data ingestion options once received
|
In Progress
|
8/15/22
|
|
Create training tools, procedure & training plan for CCO staff on how to use methodology
|
In Progress
|
8/31/22
|
|
Create procedure for updating addresses by
PH Tech staff
|
In Progress
|
8/31/22
|
If you have any questions or concerns, please contact David Ballantyne at DAVID.R.BALLANTYNE@dhsoha.state.or.us, we would love your feedback and to track any challenges you foresee. Thank you!
Effective immediately, the Oregon Health Authority (OHA) now allows the following providers to bill OHA for FDA-approved, self-collected COVID-19 home test kits supplied to FFS members on or after April 4, 2022:
- Clinic/group practices
- Critical access hospitals
- Federally Qualified Health Centers
- Home health agencies
- Hospital outpatient departments
- Independent laboratories
- Indian Health Service facilities
- Opioid treatment programs
- Physicians and other practitioners
- Rural health clinics
- Skilled nursing facilities
CCOs may choose to allow additional suppliers as described above. CCOs do not need to do this if pharmacies provide sufficient member access to COVID-19 home test kits.
OHA will cover up to 8 tests per month without prior authorization or a physician’s order, at $12 per test.
What should you do?
Providers: To bill OHA for FDA-approved or cleared over the counter test kits:
CCOs: Determine if you will allow additional providers to supply COVID-19 home test kits.
Also refer to the updated Oregon Medicaid COVID-19 Provider Guide for coverage and billing details.
Questions?
Providers: If you have any questions about this announcement, contact Provider Services Unit at dmap.providerservices@dhsoha.state.or.us or call 800-336-6016 (Option 5).
CCOs: If you have questions, please contact your CCO Account Representative.
Thank you for your continued support of the Oregon Health Plan and the services you provide to our members.
As of 8/3/2022
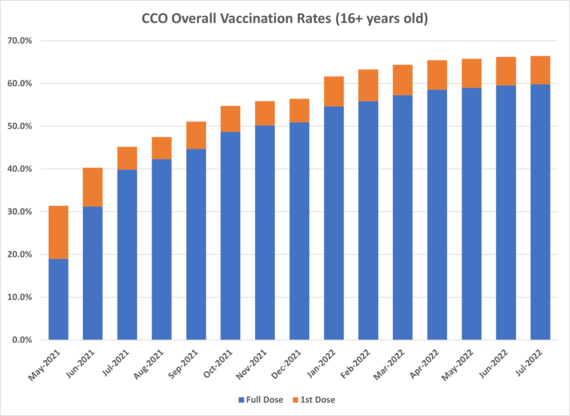 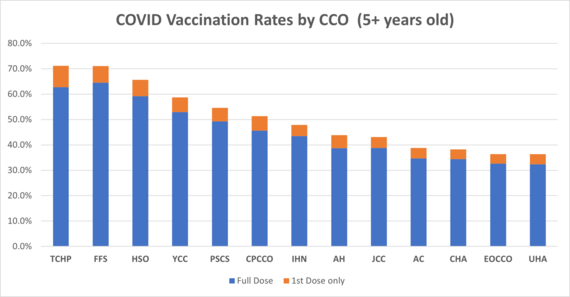
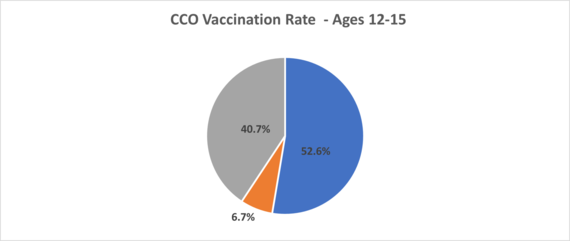 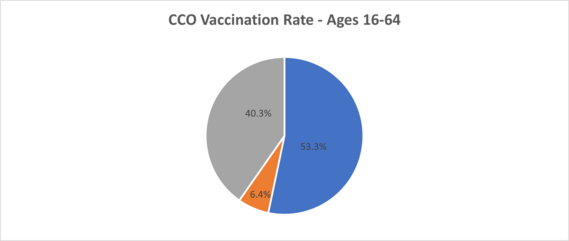 
General Overview of Final Medicaid Behavioral Health Rate Increase Proposal for Fee For Service
Thursday, August 4th @ 4:00pm – 5:00pm
Please join us for an overview of the final Medicaid behavioral health rate increase proposal for fee for service that the OHA will be submitting to CMS in mid-August. We will outline updates made in response to feedback received in early June, as well as clarify on most common questions received. Time will be held for Q&A.
An updated spreadsheet outlining the rate increase proposal, by service type and code, will be sent out ahead of time for your reference.
Medicaid behavioral health providers, payers, and partners are invited. Zoom link coming soon. For more information click here.
This abbreviated public notice provides information of public interest regarding a proposed amendment request to the federal Centers for Medicare & Medicaid Services (CMS) for the Oregon Health Plan (OHP) Section 1115 Substance Use Disorder waiver by the Oregon Health Authority (OHA).
- OHA is seeking this waiver amendment approval to implement key provisions necessary for the unwinding of the federal Public Health Emergency (PHE).
- The Section 1115 SUD waiver Bridge to the Bridge amendment will temporarily expand OHP coverage to include people in Oregon with income from 138-200% of the federal poverty level (FPL). The effective term of the proposed amendment is the end of the federal PHE. All proposed requests are subject to approval by CMS.
For more information and public meeting dates click here.
Please visit the committee and workgroup links below for more information about meetings. You can also view the OHA Public Meeting calendar.
|