|
OHA is clarifying that during the federal public health emergency (PHE), contracting with telehealth-only providers is permissible as long as a clear and timely referral process is available if a member requests in-person services.
OHA encourages the delivery of medically necessary and appropriate physical, behavioral and oral health services through live audio and video interaction between the patient and their health care provider if requested or preferred by the patient.
Why is this happening?
Per Oregon Administrative Rules (OARs) 410-141-3566 and 410-120-1990, members must have a choice between telehealth and in-person services. OHA recognizes that during the PHE, telehealth-only providers can help reduce challenges to ensure member preference and safety, network adequacy and timeliness.
Read the full memo. If you have any questions, please contact Medicaid.Programs@dhsoha.state.or.us.
The 2022 Legislature authorized the following new non-Medicaid dental programs:
-
Veterans Dental Program - Enrolled House Bill 4095
-
Compact of Free Association (COFA) Dental Program - Enrolled Senate Bill 1538
OHA expects to provide services under both new programs effective January 1, 2023.
Both bills direct OHA to contract with dental care organizations (DCOs) that serve coordinated care organization (CCO) members throughout the state and with individual oral health providers in areas not served by DCOs to provide services to eligible individuals. This direction does not take into account the following factors:
- OHA previously decided to terminate its direct contracts with DCOs at the end of 2022 and to enroll those fee-for-service members into CCOs effective January 1, 2023, under a new plan type called “CCOF.” Under this plan type, oral health services are paid for by the CCO and physical and behavioral health services are paid for by OHA’s fee-for-service program. CCOs provide oral health services to their members through a combination of subcontracts with DCOs and direct contracts with oral health providers.
- OHA’s direct contracts with DCOs are for Medicaid services, yet the services covered by the two bills are paid for with State funds only. The Centers for Medicare and Medicaid Services has final approval authority over OHA’s contracts with DCOs and does not permit non-Medicaid services to be included in Medicaid contracts. OHA does not have non-Medicaid managed care contracts with DCOs. However, OHA already has a non-Medicaid managed care contract with each CCO. The contract is for the Cover All Kids program, which will expand to the Healthier Oregon Program effective July 1, 2022. Acceptance of the non-Medicaid contract is a condition of each CCO’s Medicaid contract award; the non-Medicaid contract is substantively similar to the Medicaid contract, save the source of funds used to pay the CCOs.
OHA has determined, consistent with the legislative intent of HB 4095 and SB 1538, to enroll the individuals eligible for oral health services in CCOs in the “CCOF” plan type and to have those services administered by the CCOs under their non-Medicaid managed care contracts.
OHA will communicate with CCOs about implementation of the two new dental programs over the coming months. Draft contract language and payment rates for the non-Medicaid contract will be provided to CCOs by September 16, 2022, consistent with the schedule previously provided by OHA to CCOs.
Read the full memo. If you have general questions about this, please contact Cheryl Henning, CCO Contracts Administrator and Interim DCO Contracts Administrator, at Cheryl.L.Henning@dhsoha.state.or.us.
OHA missed updating OAR 410-141-3830 to correctly reference the 1/1/2022 Prioritized List of Health Services. A temporary rule was filed to correct this oversight.
- The rule reference was incorrect from 1/1/2022 to 4/15/2022. It incorrectly referenced the past list when it should have been updated to reference the 1/1/2022 list.
- The web link in the rule was correct.
- Operational changes that depend on the list such as CCO rate development and capitation were not affected.
What should you do?
- Confirm that you are using the 1/1/2022 list for operations and that you were using it effective 1/1/2022. The list is commonly used in claims processing and by prior authorization reviewers.
- For cases with dates between 1/1/22 – 4/14/22 that rely on the Prioritized List, you may site this retroactive rule if needed.
Why is this happening?
OHA strives to keep all our OARs current, but we unfortunately missed the update for 1/1/2022. We regret the error.
Read the full memo. If you have questions about this announcement, please contact your CCO Account Representative.
Fee-for-service rate increase for newborn bloodspot screening kits, effective September 1, 2021
OHA has increased the fee-for-service reimbursement rates for the newborn bloodspot screening kit (supply code S3620). For services provided on or after 9/1/2021:
- The rate for the two-part kit is $80.00.
- The rate for a replacement kit containing one part only is $59.00 (add modifier TC to code S3620).
- OHA will accept separate billing for the kits (outside of the bundled rate for newborn delivery).
The next publication of the Oregon Health Plan (OHP) fee-for-service fee schedule will reflect the increase.
The increase applies only to claims billed to OHA by enrolled OHP providers for members not enrolled in a CCO. Read the full memo.
Increased fee-for-service dispensing fee, effective July 1, 2022
OHA is increasing reimbursement for CPT code 92340 (fit spectacles monofocal) to $130.00. This increase becomes effective on July 1, 2022.
Once prescribed glasses, Oregon Health Plan members must often search for a provider who will fit and dispense them, sometimes across several counties. In researching this issue with several providers, we found that the rate was too low for this service. Read the full memo.
OHA is convening a workgroup to provide feedback on 1115 waiver policy and implementation of the social determinants of health (SDOH) benefits for members in transition populations. The CCO feedback will inform OHA negotiations with CMS, as well as implementation of the final, approved waiver, along with feedback from the community and other stakeholders.
When: The workgroup will begin meeting in July and will meet weekly to start.
How to join: Please email Anona Gund at anona.e.gund@dhsoha.state.or.us to be added to our list.
Oregon’s Joint Task Force on Universal Health Care invites you to its regional community listening sessions to listen, learn, and provide feedback about its work so far. Please download and share the invitation.
-
Southern Region | Saturday, June 18 - 10:30 am to 12:30 pm - Zoom link: shorturl.at/pvxRX
-
Portland Metro | Tuesday, June 21 - 5:30 pm to 7:30 pm - Zoom link: shorturl.at/uDGQ4
-
Willamette Valley | Saturday, June 25 - 10:30 pm to 12:30 pm - Zoom link: shorturl.at/rGJZ2
Learn more about the Task Force on Universal Health Care.
The Measure 110 Oversight and Accountability Council (OAC) approved Behavioral Health Resource Networks (BHRNs) in eight additional Oregon counties this week. The OAC approved BHRNs in Benton, Columbia, Crook, Hood River, Marion, Polk, Umatilla and Washington counties.
The funds for the 18 approved BHRNs total more than $71 million. To date, approximately $113 million has been allocated in support of Measure 110, including Access to Care (ATC) grant funding.
OHA has developed a statewide map visualization showing the BHRNs that have been approved for funding; (in orange) along with those that have been selected by the OAC (in blue) and are in negotiations for funding approval.
OHA has also established a robust new dashboard showing the BHRN approval and funding progress being made to date. OHA will continue to provide frequent updates on the funding process. Read the full news release.
New rules that go into effect July 1 will require health care providers reimbursed with public funds to work with credentialed health care interpreters qualified or certified by OHA.
The rules drafted by OHA reflect changes in the requirement for health care interpreting services in Oregon that were made by the state Legislature’s passage of House Bill 2359 during the 2021 session. These new rules will ensure that people for whom English is a second language (those with limited English proficiency) or who use sign language can access high-quality interpreting services so they can receive health care like anyone else in Oregon. This access is critical to achieving the state’s mission of eliminating health inequities by 2030.
Read the full news release. For more information about HB 2359, OHA’s central registry or health care interpreter services, visit the Health Care Interpreter Program website.
Weekly updates on major Medicaid projects
1115 Medicaid Waiver
The current 1115 Waiver ends June 30, 2022. OHA anticipates an extension until September 30, with approval for the renewal at that time.
***
Oregon Health Plan Redeterminations
No new updates.
***
Healthier Oregon
FAQ
A new Frequently Asked Questions document has been shared, which includes information about program eligibility, benefits, outreach and impacts. To learn more, visit Oregon.gov/HealthierOregon or Oregon.gov/OregonMasSaludable.
Office hours
Please note that the final Healthier Oregon Office Hours is:
Tuesday, June 21st, 12:30 – 1:30 PM
Click here to join the meeting
Or call in (audio only) +1 971-277-2343,,771570543#
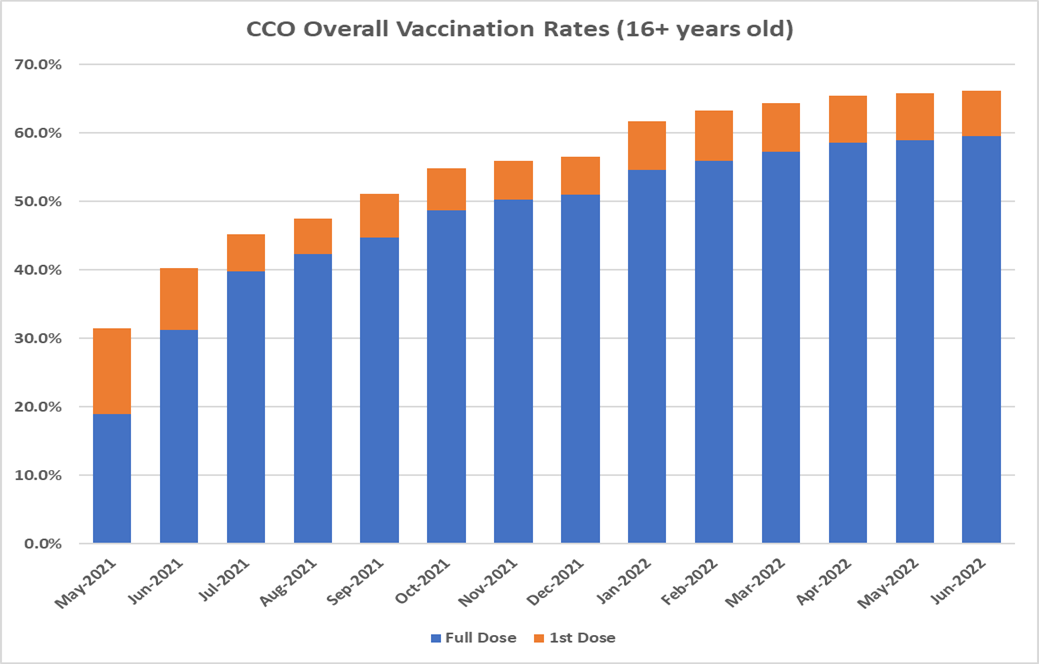
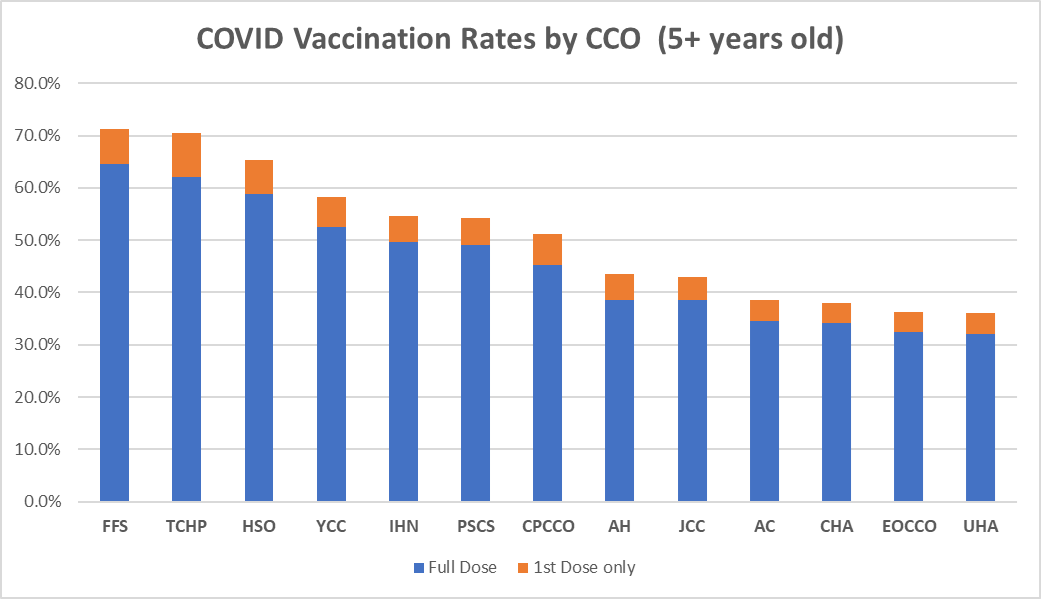
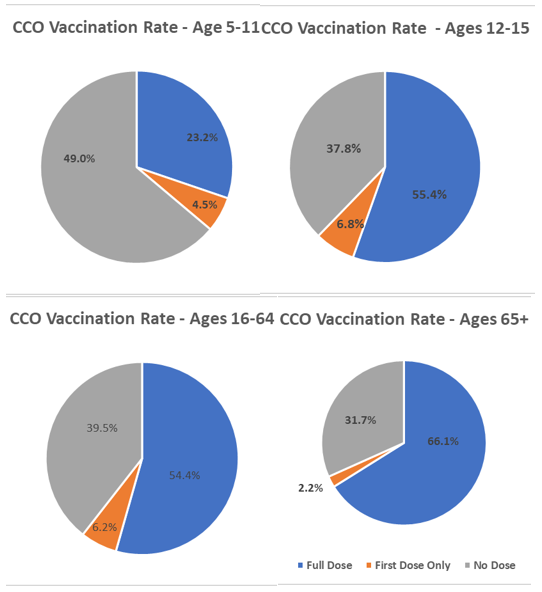
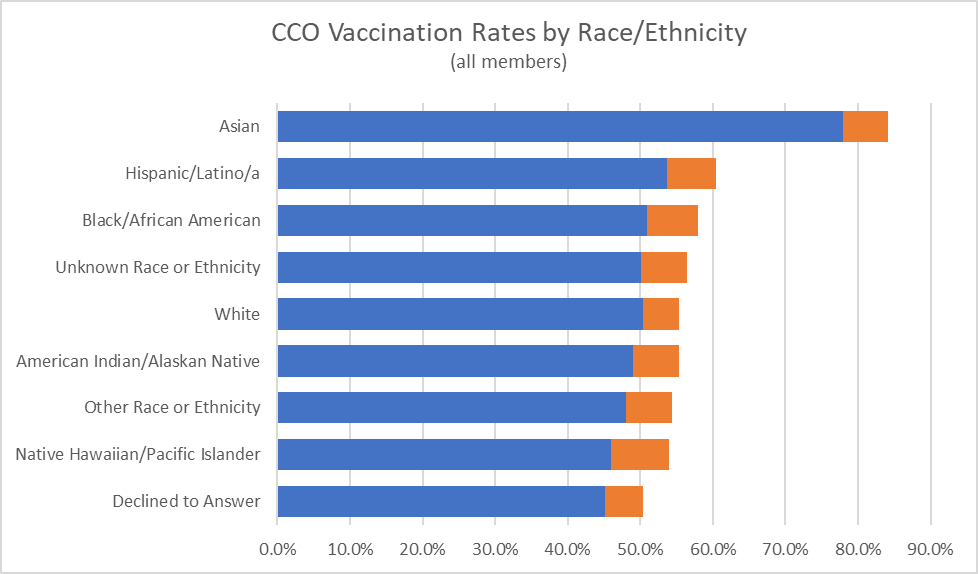
Rates as of 06/15/2022
June 21, 2022
June 24, 2022
- 9 a.m. to 12 p.m., Metrics & Scoring Committee
-
Agenda includes: Public testimony, Draft 2023 Challenge Pool, Groundwork for new measurement structure centered on Equity
Please visit the committee and workgroup links below for more information about meetings. You can also view the OHA Public Meeting calendar.
|