April 2026
Reminder that the provider attestation requirement related to amended Executive Order 2025-16, is due by May 15, 2026. The updated provider attestation form is available under Forms on OHCA's Provider Enrollment page. View FAQs for additional info and submission instructions, or contact ProviderEnrollment@okhca.org or 800-522-0114, option 5, with questions.
Earlier this year, OHCA hosted a series of SoonerSelect town halls across the state to answer your questions and hear your feedback. From those sessions, we aggregated common questions into a frequently asked questions document. You can find the FAQ document on OHCA's SoonerSelect provider webpage in the Quick Links sidebar.

The SoonerSelect 2026 open enrollment period runs from May 1-June 12. During this period, encourage your patients to visit the SoonerSelect page and review their health and dental plans, along with the extra benefits offered by each.
SoonerSelect members can change either their health plan, dental plan or both. If they’re happy with their current plans, they don’t need to do anything.
Members can change plans online at MySoonerCare.org or by calling the choice counseling line at 800-987-7767, option 5. Changes must be completed by June 12, 2026.
If you would like free SoonerSelect open enrollment posters for your clinic or office, you can order them here. They are available in English and Spanish.
|
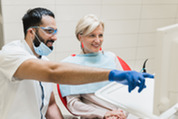
Dental coverage applies to members who are:
- Receiving dental services through the Homeward Bound Waiver.
- Age 21 and older receiving dental services through the Community Waiver or In-Home Supports Waiver for adults.
Dental services include services per OAC 317:30-5-482. Preventive, restorative, replacement and repair services to achieve or restore functionality are provided after appropriate review, when required per OAC 317:40-5-112(e). View OHCA’s policies and rules regarding dental services for members in a waiver program.
All arrangements for services must be made with the Developmental Disabilities Services (DDS) case manager and be specified in the member's individual plan.
Requests for preauthorization must propose services that are the most cost effective to restore dental health.
For further assistance, contact the Oklahoma Department of Human Services within the member's residential county.
The OHCA dental team may be reached at 405-522-7401. For faster assistance, please email DentalServices@okhca.org.
|

Did you know that when a provider brings up smoking and recommends quitting, the chances of successful long-term cessation double? A brief, direct question can move your patient from “not today” to “maybe it's time.” Your voice is one of the strongest prompts for a quit attempt.
April is Stress Awareness Month, and stress is one of the most common reasons patients give for continuing to smoke. But nicotine can increase anxiety over time. Smoking rates also remain higher among patients with behavioral health conditions, making consistent screening even more important.
The Oklahoma Tobacco Helpline is built to support the work you start. Patients can access free nicotine replacement therapy (if eligible), one-on-one coaching and ongoing support beyond the exam room. Referral options are designed to fit into your existing workflow, and free educational materials are available to reinforce the message in your office.
The Oklahoma Tobacco Helpline is here to help your patients quit and improve their health outcomes. And don't forget to stock your office with free Helpline materials like pens, brochures and prescription pads. Order online today.

The State of Oklahoma is holding a town hall to review upcoming electronic visit verification (EVV) changes. It will include updates on the current vendor (Authenticare), the SoonerSelect vendor (HHAX) and the state’s transition from Fiserv’s Authenticare to Acumen’s Direct Care Innovations (DCI).
The town hall will be held on Zoom at 2 p.m., Tuesday, May 19. Register to watch. Entities involved in EVV compliance and oversight, including provider agency leaders and workers, and case managers, are encouraged to attend.
Additional guidance on timelines, training and support will be released in the coming months. Provider agencies should monitor these updates closely to ensure leadership, case managers and EVV oversight staff are prepared for the transition.
|

Provider Files
Please update your OHCA provider files to ensure all details, including new or missing locations and group member assignments, are accurate. If your update impacts services under SoonerSelect partners, email your Application Tracking Number (ATN), received upon submitting your update on the OHCA provider portal, to ProviderEnrollment@okhca.org with "SoonerSelect update" and your ATN in the subject line.
Renewal Processing
Due to the high volume of renewals, processing is taking longer than usual. OHCA published a global message on Feb. 2, informing providers that renewals have been extended to April 30, 2026.
Provider types for case management agency, personal care agency, self-directed support and services, assisted living, Advantage home-delivered meal, pharmacy and DME are being extended to May 31, 2027, as noted in the April 6 and April 9 global messages.
Provider types for podiatrist, physical therapist, speech/hearing therapist, occupational therapist, audiologist, dietitian, ambulance and air ambulance are being extended to Aug. 31, 2026, as noted in the April 14 global message.
Please ensure your contact information, including email address, is up to date for all individual and facility/group provider files so you receive important contract information.
Provider Renewals
For the following provider types, 75-day renewals started March 15, and contracts expire May 31, 2026:
- Behavioral health practitioner under supervision
|
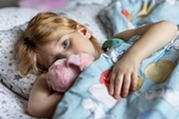
A recent study showed an average of 22 adolescent deaths each week from drug overdoses in the United States, making overdose/poisoning the third-leading cause of pediatric deaths. These trends highlight the importance of evidence-based prescribing. Recent guidelines emphasize strategies that prioritize safety and adequate pain control.
Consistent use of validated pediatric pain assessment tools — including FLACC, Wong-Baker FACES and numeric rating scales — can support individualized treatment and help reduce unnecessary opioid exposure.
If you have questions about a particular medication, or other pharmacy benefit questions, please call the Pharmacy Help Desk associated with your patient’s health plan.
|

SoonerCare offers Diabetes Self-Management Education and Support classes to members that have been diagnosed with type 1 and II diabetes. These classes can help your patients with eating healthier, medical adherence, being more active and checking their glucose level, along with other educational topics and resources that will help with managing their diabetes.
|

SoonerCare offers a variety of ways to help your patients along their quit journey to quit for good. The tobacco cessation benefit includes:
- All six FDA-approved tobacco cessation medications that do not count against a member’s six-prescription limit per month.
- Tobacco cessation counseling session with their SooneCare provider.
- Services with the Oklahoma Tobacco Helpline.
Current or former tobacco smokers can also take advantage of a low-dose lung cancer scan that can assist in early detection of cancer. Early screening and detection can decrease cancer mortality by 14% to 20%.
|

Does a progress note need to be tied to an actual encounter?
All prior authorization requests for therapy services should be submitted in a timely fashion following completion of an evaluation or progress note. These notes are the basis by which determinations are made regarding a member’s current medical need for the skilled service.
For any continuation request within the year of an evaluation, a progress note is required to provide justification of medical necessity. Progress notes can show a continued need for treatment by ascertaining goal progress, confirming changes due to rendered services, recognizing changes due to gaps in services, and creating a cohesive record of the member to date. This note can also be useful for purposes of handoff in a change of provider situation.
For PT/OT or SLP, when a progress note is required for a PA request, it should be tied to an encounter, and relevant measurements should be conducted during the encounter. Progress note visits should, at a minimum, include this information for PT/OT and SLP: subjective and objective measures showing current progress toward established and relevant goals with a detailed commentary provided.
Below is an example:
Goal: Member will elicit ability to perform a single leg hop for at least 75cm for the R. LE by 6 months without compensatory movement patterns suggesting good synergistic LE muscle activation for a safe return to age-appropriate activities and participation in high school basketball.
Current Progress: Continue, pt does not meet this goal as written.
The commentary above does not elaborate on goal progress or show a continued need for skilled intervention. However, the commentary provided below meets these requirements.
Current Progress: Continue, member demonstrated ability to perform SL hop safely at almost 6 months post-op today; member can perform 55 cm with mild upper body swaying present eliciting continued need to improve plyometric strength and synergistic LE stabilization when landing; Prognosis: excellent with continued coverage over the next auth period.
What should I enter under the “Service Provider Information” section of the OHCA prior authorization portal?
When submitting a PA request in the provider portal, you must enter mandatory information by the section.
- Enter the provider ID in the “Requesting Provider Information” section.
- Enter the Member RID number in the “Member Information” section.
- When you reach the “Service Provider Information” section, do not fill out this section. Entering information in this section will create issues when filing claims leading to a denial of reimbursement.
The process above should be applied for any therapies PA request submission for members under 21 years old.
When is a Change of Provider form necessary for a PA request?
A Change of Provider (COP) form is necessary when services are transferred from one clinic/location to another (parental signature showing that services will no longer be conducted under the originally approved provider ID). The previous clinic is responsible for ensuring an appropriate handoff to the new clinic with provision of the referring provider’s order and an up-to-date progress note. The new clinic is responsible for a timely PA submission meeting all documentation requirements.
As CPT codes themselves cannot be approved at two different locations simultaneously, it is important to note that a COP form could be necessary more than once. For example, if an SLP eval PA request for CPT 92523 is submitted with a COP form and it is approved, then the subsequent SLP treatment PA request for CPT 92507 must also include the COP form.
Do I need to submit a PA request if Medicaid is not the member’s primary coverage?
Medicaid is always the payor of last resort. When Medicaid is a secondary form of coverage for a member, it is required that a PA request be timely submitted with all necessary documentation for all PA-requiring services. This ensures continuation of coverage whenever the primary insurance stops covering the service for any reason.
The only exception to this need to timely submit a PA is when the primary insurance is Medicare. In such situations, when Medicaid is not the primary and Medicare is, a PA submission is not necessary as a claim can be submitted to Medicaid as a crossover claim whenever Medicare coverage is exhausted.
|
|
Chief Executive Officer
Clay Bullard
OHCA Board of Directors
Marc Nuttle, Chairman
Norman, OK
Alex Yaffe, Vice Chairman
Oklahoma City, OK
Tanya Case
Duncan, OK
John Christ
Oklahoma City, OK
Kevin Corbett
Edmond, OK
Jeffrey Cruzan, M.D.
Oklahoma City, OK
Clark Jolley
Edmond, OK
Kim Leland
Norman, OK
Phillip Kennedy
Lawton, OK
Information contained within this newsletter is subject to change. Be sure to check OHCA provider letters, global messages and web alerts at OKHCA.org for the most up-to-date information.
Our vision is for Oklahomans to be healthy and to have access to quality health care services regardless of their ability to pay.
OHCA Core Principles:
Passion for Our Purpose
Empowerment and Accountability
Trust and Transparency
Solution-oriented
Servant Leadership
The Oklahoma Health Care Authority does not discriminate on the basis of race, color, national origin, sex, religion, age or disability in employment or the provision of services.

|











