Appendix K Waiver Amendment - Attention Referring Providers: Enhancement to KEPRO’s Referral Management Process for Family Choice Members ONLY - April 2020 Drug Rate Updates
Maine Department of Health & Human Services sent this bulletin at 05/11/2020 12:38 PM EDT Having trouble viewing this email? View it as a Web page.
Having trouble viewing this email? View it as a Web page.
DHHS Receives Federal Approval of Appendix K Waiver Amendment
On May 8, 2020, the Centers for Medicare and Medicaid Services (CMS) approved DHHS’ Appendix K waiver amendment. As announced on April 30, the DHHS Offices of MaineCare Services and Aging and Disability Services submitted an Appendix K waiver amendment requesting the flexibility to temporarily increase support to providers of home- and community-based services for more than 5,600 adults with physical or intellectual disabilities, brain injuries and other related conditions, and older Mainers.
Approval of this waiver gives MaineCare the flexibility to increase reimbursement rates by 10% for the most highly utilized direct care services for these populations, with the expectation that providers will use most of this financial relief to retain and support their direct care staff, such as by offering hazard pay. The increase, totaling nearly $13 million in state and federal funds, will be retroactive to March 1, 2020 and continue through May 2020.
Approval of this amendment also:
- Allows relatives or spouses to provide services and receive payment, when hired or contracted by a provider agency
- Increases reimbursement for home-delivered meals, from one meal a day to two
- Reimburses providers for taking steps to safely isolate COVID-19 positive residents, either in their existing facilities or in separate facilities, in accordance with U.S. CDC guidelines
- Allows shared living settings to expand to up to three individuals
- Encourages the use of telehealth to fill service gaps when people cannot be served face-to-face
- With DHHS approval, allows members to exceed some service limits, including hours of service provided and charges relating to assistive technology, to promote use of telehealth
- Allows services to be provided in alternative settings (e.g. hotels, shelters, schools, churches, etc.) when necessary to respond to the COVID-19 crisis.
This will impact the following MaineCare waiver programs:
- Section 18, Home and Community-Based Services for Adults with Brain Injury
- Section 19, Home and Community Benefits for the Elderly and Adults with Disabilities
- Section 20, Home and Community-Based Services for Adults with Other Related Conditions
- Section 21, Home and Community Benefits for Members with Intellectual Disabilities or Autism Spectrum Disorder
- Section 29, Support Services for Adults with Intellectual Disabilities or Autism Spectrum Disorder
MaineCare will be issuing provider guidance on the implementation of these provisions in the near future. For more information, please see CMS’ approval letter and the Appendix K waiver application.
Attention Referring Providers: Enhancement to KEPRO’s Referral Management Process for Family Choice Members ONLY
Effective Monday, May 11, 2020, the Office of Children and Family Services (OCFS), in coordination with KEPRO, will implemented changes in the referral management process.
In an effort to improve the referral process for both Home and Community Treatment and Rehabilitative Community Services, KEPRO has developed a new Family Choice Waitlist report that is accessible in the KEPRO Atrezzo System. The report will display all consumers who have been added to the Family Choice Waitlist by KEPRO and are waiting for services from your agency that have not been served.
How to find your agency’s Family Choice Waitlist Report
Step 1: Login to KEPRO’s Atrezzo Portal at https://atrezzo.kepro.com/.
Step 2: Select PROVIDER REPORTS in the menu bar. Please note: the Provider Reports tab is only available to users with a Group Admin +Reports or Admin +Report user role in Atrezzo.
![]()
Step 3: Click the report named Family Choice Waitlist.
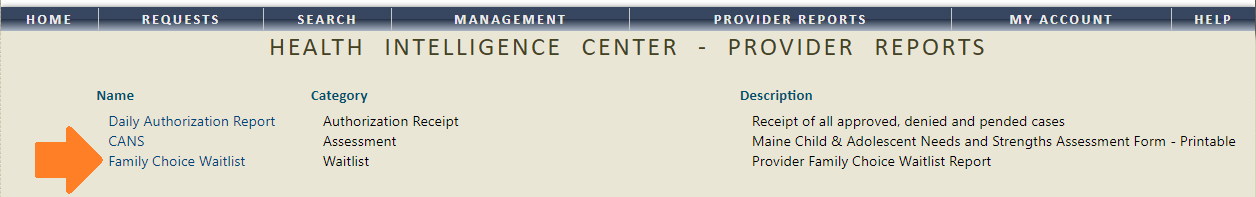
Step 4: Enter the report parameters and click View Report.
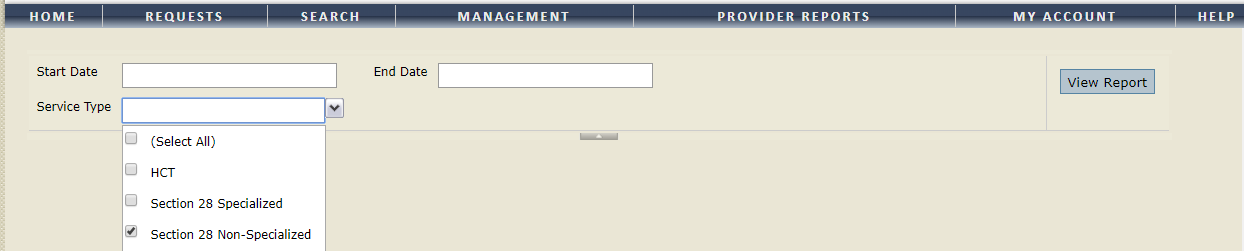
The report will be displayed below. Please note: The report may be exported as an Excel file by clicking the save button ![]()
Family Choice Providers
KEPRO will match children to the appropriate services and agency based on the longest wait days. If the referral source indicates a preferred provider on the referral management questionnaire, and the caregiver would like to continue to wait for preferred provider, KEPRO will move the referral to the preferred agency with the appropriate NPI number (listed below). This referral will now become part of the agency’s Internal Family Choice Waitlist. It is the expectation that the agency to serve the member as soon as they have capacity.
Example of the Referral Management Questionnaire Preferred Provider/Family Choice List

Instructions Availability
This instructional information will be available on the Provider Resources webpage for future reference.
Questions?
Please contact KEPRO with questions at IntakeME@kepro.com.
Drug Code Rate Updates, CR 94345
Effective April 29, 2020, Drug code rates were revised in MIHMS retroactive to April 1, 2020 due to Centers for Medicare and Medicaid Services (CMS) rate update. Affected claims will be reprocessed and no provider action is needed. See the updated April 2020 Drug Rates (PDF) for more detail.
