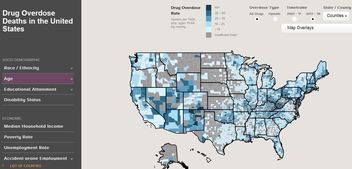
 The National Opinion Research Center at the University of Chicago and the U.S. Department of Agriculture have created an online tool to allow users to map overdose hotspots and overlay them with data that provide additional context to opioid addiction and death - including the strength and diversity of local economies, ethnicity, educational attainment and disability status of residents. The tool utilizes data between two timeframes, 2007-2011 and 2012-2016, which can be broken down by state and even by county.
The American Medical Association’s Opioid Task Force encourages physicians to consider co-prescribing naloxone with opioids when it is clinically appropriate to do so, such as in cases where the patient may have a history of substance abuse or the patient has a concurrent benzodiazepine prescription. Though co-prescribing naloxone is not a guarantee for an overdose reversal, it does provide a tangible option for care that otherwise may not be available in a timely manner. Co-prescribing naloxone is supported by a broad range of organizations, including the World Health Organization, U.S. health agencies (CDC, SAMHSA), and many patient, consumer and other advocacy groups.
 |
A new paper published in the journal Addictive Behaviors highlights the intersection between traumatic brain injury (TBI) and the opioid epidemic. It is estimated that 20 percent of non-institutionalized adults have experienced at least one TBI with a loss of consciousness during their lifetime. It has been demonstrated that survivors of TBI are at risk for problem substance use, post-injury. Practitioners can proactively mitigate potential opioid use problems by identifying high-risk populations, which includes individuals with a history of TBI. Clinicians considering initiation of opioids for pain should complete an evaluation of a patient's history of TBI and follow existing clinical guidelines when prescribing opioids.
Dayton, Ohio, had one of the highest opioid overdose death rates in the nation in 2017 and the worst in Ohio. The city made many changes, and fatal overdoses are down more than 50 percent from the previous year. Changes included expanding Medicaid to give more low-income adults access to free addiction and mental health treatment, increasing the availability of naloxone and developing better post-treatment support.
|