 This update is being sent to members of the Wisconsin Travel Health Network.
Global Health Update
Nipah virus outbreak in India, Marburg outbreak ended
The Nipah virus is causing a small outbreak in India. Two nurses were initially infected in West Bengal. Health officials traced 196 contacts, all of whom have been quarantined and tested negative. Nipah spreads through direct contact with bodily fluids, and the virus lives primarily in animals. As spillover events are rare and the virus does not easily spread from person to person, public health risk is low at this time.
Additionally, the Marburg virus disease outbreak in Ethiopia that started on November 14 was declared over on January 26. Find more information about the outbreak here.
CDC Travel Health Notices for international travelers
Level 4—Avoid All Travel
None at this time.
Level 3—Reconsider Nonessential Travel
None at this time.
Level 2—Practice Enhanced Precautions
Chikungunya in Bolivia (2/11/2026), Seychelles (2/5/2026) and Suriname (2/17/2026)
There are outbreaks of chikungunya in Boliva, Seychelles, and Suriname. Travelers to these areas should take steps to avoid mosquito bites.
Clade II mpox in Ghana and Liberia (1/26/2026)
There are outbreaks of clade II mpox in Ghana and Liberia. Mpox is endemic in these countries. These outbreaks have affected males and females approximately equally. Mpox vaccination with the JYNNEOS vaccine is recommended for travelers to these countries who anticipate certain sexual activities.
Level 1—Practice Usual Precautions
Global Dengue (1/22/2026)

Spring break travel reminders
Spring break is at the end of March for most Wisconsin schools. Students and their families traveling during this time should keep these travel health tips in mind to make sure they have a safe and healthy vacation.
-
Sun exposure: Remind travelers to protect themselves from the sun by using sunscreen with a sun protection factor (SPF) of 15 or higher, reapplying their sunscreen every two hours and after getting out of water, and wearing protective clothing like wide-brimmed hats and sunglasses.
-
Bug bite prevention: Individuals traveling to areas with mosquito and tick activity should pack insect repellant with 20–30% DEET, 10–20% picaridin, 10–20% IR3535, or 30–40% oil of lemon eucalyptus on skin and clothes to prevent bug bites. Encourage travelers to wear long-sleeved shirts and pants if they are traveling to locations with mosquito-borne illness transmission.
-
Food safety: Travelers should avoid eating raw and street foods to lower their risk of consuming contaminated food.
-
Freshwater germs and parasites: Freshwater can contain parasites, bacteria, and viruses that cause diarrhea and skin infections, even if the water looks clean. Travelers should be wary of swimming in lakes and rivers where parasites are common. Brazil, Egypt, Southern China, sub-Sarhan Africa, the Philippines, and Southeast Asia are areas where bodies of water can contain parasites.
|

Traveler-Based Genomic Surveillance Program Surpasses One Million Participants
On January 30, the Center for Disease Control and Prevention (CDC)'s Traveler-Based Genomic Surveillance (TGS) Program surpassed one million voluntary air travel participants. Launched in 2021, TGS is a tool used to strengthen disease surveillance at U.S. airports. Through voluntary, anonymous nasal sample collection from arriving international travelers, the program provides early insight into emerging pathogens before they spread throughout the country. TGS detects variants of seasonal respiratory viruses and other pathogens of public health concern; for example, the program reported the first two detections of influenza H3N2 subclade K in the U.S. In addition to nasal samples, CDC also analyzes airplane wastewater samples as part of its biosurveillance efforts. Learn more about the program and TGS data.
|
Disease Spotlight: Meningococcal Disease
Meningococcal disease is caused by Neisseria meningitidis, a gram-negative diplococcus bacterium. Meningococci are classified into serogroups based on the composition of their capsular polysaccharide. The six major meningococcal serogroups associated with disease are A, B, C, W, X, and Y. Someone with meningococcal disease can have meningitis, sepsis, or both at the same time. Anyone can get meningococcal disease, but it is most common in children under 5 years of age and young adults ages 16–23 years.
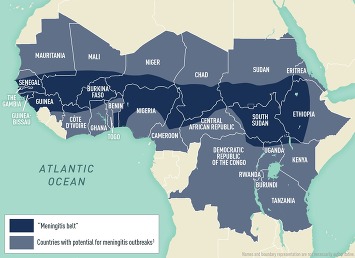
N. meningitidis is found worldwide, but incidence is greatest in the "meningitis belt" of Sub-Saharan Africa. Meningococcal disease is hyperendemic in this region, and periodic epidemics during the dry season (roughly December–June) reach an incidence of up to 1,000 cases per 100,000 population. By contrast, rates of disease in Australia, Europe, South America, and the United States range from 0.1–2.4 cases per 100,000 population per year.
N. meningitidis bacteria are often found in the nose and throat without causing illness. Most people who come into contact with N. meningitidis do not get sick. Only some people become seriously ill, which may be related to societal factors such as overcrowding or smoke exposure, or physical factors such as a weakened immune system that make them more likely to get sick.
|
How is it spread?
Meningococci spread through respiratory secretions and require close contact for transmission. Both asymptomatic carriers and people with overt meningococcal disease can be sources of infection. Asymptomatic carriage is transient and typically affects approximately 5–10% of the population at any given time.
Who is at risk?
Unvaccinated travelers visiting meningitis belt countries and having prolonged contact with local populations during an epidemic are at greatest risk for meningococcal disease. The Hajj and Umrah pilgrimages to Saudi Arabia also have been associated with outbreaks of meningococcal disease among returning pilgrims and their contacts, including six cases in Umrah participants and their contacts in the United States in 2024.
Is a vaccine available?
Yes, six meningococcal vaccines are licensed and available in the United States. The American Academy of Pediatrics (AAP) recommends routine administration of a quadrivalent meningococcal conjugate vaccine (MenACWY) series for all people aged 11–18 years. Administer a single dose of vaccine to patients at age 11 or 12 years and a booster dose at age 16 years. ACIP also recommends that adolescents and young adults aged 16–23 years be vaccinated with a serogroup B meningococcal (MenB) vaccine series.
For travelers to countries where meningococcal disease is hyperendemic or epidemic, a dose of one of the four MenACWY vaccines (Menveo®, MenQuadfi®, Penbraya®, and Penmenvy®) is recommended, in accordance with this schedule. Travelers should receive vaccination at least 7–10 days before travel to enable time for protective antibody levels to develop.
What are the symptoms?
Meningococcal disease generally occurs 1–10 days after exposure and presents as meningitis in approximately 50% of cases in the United States. Meningococcal meningitis is characterized by sudden onset of headache, fever, and neck stiffness, sometimes accompanied by nausea, vomiting, photophobia, or altered mental status. Approximately 30% of people with meningococcal disease present with meningococcal sepsis, known as meningococcemia. Symptoms of meningococcemia can include abrupt onset of fever, chills, vomiting, diarrhea, and a petechial or purpuric (non-blanching, flat) rash, which can progress to purpura fulminans (a disorder where skin bleeds and dies rapidly).
Meningococcemia often involves hypotension, acute adrenal hemorrhage, and multiorgan failure. An additional 15% of meningococcal disease cases in the United States, primarily among adults older than 65 years of age, present as bacteremic pneumonia.
Other presentations (such as septic arthritis) also occur. Among infants and children under 2 years of age, meningococcal disease can have non-specific symptoms. Neck stiffness, usually seen in people with meningitis, might be absent in this age group.
Meningococcal disease progresses rapidly and has a case-fatality rate of 10–15%, even with antimicrobial drug treatment. Without rapid treatment, fatality rates can be much higher. In addition, up to 20% of survivors can have long-term health effects such as deafness or amputations due to necrosis of the extremities.
How is it diagnosed?
Early diagnosis and treatment are critical. If bacterial meningitis is suspected, collect blood for culture right away and perform a lumbar puncture (LP) to collect cerebrospinal fluid (CSF) for microscopic examination and Gram stain. In general, diagnosis is made by isolating N. meningitidis from a normally sterile body site like blood or CSF either by culture or by PCR detection of N. meningitidis-specific nucleic acid. The Wisconsin Department of Health Services (DHS) can provide diagnostic and testing support if needed.
Signs and symptoms of meningococcal meningitis are like those of other causes of bacterial meningitis (including Haemophilus influenzae and Streptococcus pneumoniae). Proper treatment and prophylaxis depend on correctly identifying the causative organism. Meningococcal disease is nationally notifiable in the United States; report cases to DHS without delay.
Are there treatments?
Meningococcal disease can be rapidly fatal and should always be viewed as a medical emergency. The priority in management of meningococcal disease is treatment of shock in meningococcemia and of raised intracranial pressure in severe meningitis. As soon as disease is suspected and blood cultures and CSF have been collected, deliver appropriate treatment. If the LP is to be delayed for any reason, administer antimicrobial drugs immediately after collecting blood cultures. Begin empiric antimicrobial drug treatment early and prior to receiving diagnostic test results.
Third-generation cephalosporins (cefotaxime or ceftriaxone) are recommended for empiric treatment. Determine meningococcal isolate susceptibility before switching to penicillin or ampicillin; recent reports indicate emerging penicillin resistance among meningococcal isolates in the United States. If a patient presents with suspected bacterial meningitis of uncertain etiology, some treatment algorithms recommend empiric use of dexamethasone in addition to an antimicrobial drug until a bacterial etiology is established; if meningococcal meningitis is confirmed or suspected, steroids can be discontinued.
Due to detection of ciprofloxacin-resistant strains of N. meningitidis, Wisconsin is under a two-year restriction for ciprofloxacin use. Providers should prescribe ciprofloxacin alternatives as prophylaxis.
How can it be prevented?
The best way to prevent meningococcal disease is to get the recommended vaccines for travelers to countries where meningococcal disease is hyperendemic or epidemic and to avoid kissing or sharing cups, utensils, with someone who is sick.

In case you missed it: Managing Histoplasmosis in Returning Travelers
The Centers for Disease Control and Prevention (CDC) held a webinar about travel-associated histoplasmosis on January 15. Watch a recording of the webinar.
|
|