Oregon House protects health coverage
Oregon Department of Human Services sent this bulletin at 06/16/2017 03:30 PM PDT
Update on Medicaid eligibility clean-up
Last week OHA shared an update on plans to complete the last stages of Medicaid eligibility clean-up with the Governor and legislators. The data clean-up plan was approved by the federal Centers for Medicare & Medicaid Services (CMS) in 2015.
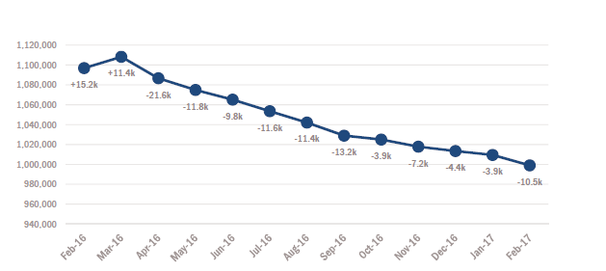
As of May 1, 2017, more than 733,600 Oregon Health Plan (OHP) members have been found eligible to continue receiving OHP coverage. We are finalizing the eligibility renewal process for a remaining 115,236 cases. These remaining cases have been housed in older databases. They were triaged for the final stage of the Medicaid clean-up due to their complexity. Here are some of the programming challenges this week’s analysis identified:
The clean-up process will be completed by August 31, 2017.
At that time all Medicaid case renewals will be in the ONE system and on an up-to-date renewal cycle. You can review Director Saxton’s presentation on this topic to the Senate Health Care Committee here.
 Oregon moves to centralize benefit eligibility processing
This week OHA Director Lynne Saxton and Department of Human Services (DHS) Director Clyde Saiki shared the following announcement with OHA and DHS employees and community partners:
Earlier this year we announced our agencies were convening a project team to explore the centralization of financially based benefit eligibility decision-making between our agencies – i.e., integrating TANF, SNAP, Medicaid and other benefits for effectiveness and efficiency. We want to provide you an update on the Integrated Eligibility/Medicaid Eligibility (IE/ME) project.
Our agencies share a commitment to provide Oregon families access to the services and supports they need to lead healthy and productive lives. More than 60 percent of the people to whom OHA provides Medicaid services also receive benefits or services from DHS. The goal of integrated eligibility is to centralize and streamline the benefit eligibility process to make it more efficient and easier to navigate for our clients.
As part of this vision, we intend to centralize the Medicaid eligibility determination process:
The first steps in this long-term vision is centralizing Medicaid eligibility at DHS later this year. While this transition is underway, OHA will continue to administer the Medicaid eligibility process.
The IE/ME project team is still early in the planning and implementation process and we are working partners. This transition will require changes in organizational structure, reporting and staffing – e.g., OHA’s Member Services team will move to DHS in coming months as part of this transition.
Both agencies are working closely together to carry out a collaborative transition process that minimizes disruption for clients and staff and provides adequate and appropriate training, technology and support.
Our shared goal of providing
effective and efficient health and social services is at the heart of this
transition. We appreciate your partnership in improving the lives of
Oregonians.
|