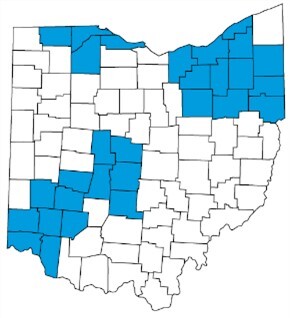
The Ohio Department of Medicaid (ODM) implemented the Next Generation MyCare program today. The program is available in 29 Ohio counties. Later in the year, it will be available in the rest of Ohio.
Thank you for helping us prepare for the Phase 1 Roll Out and supporting Ohioans’ healthcare needs. Please continue to spread the word and be ready to answer member and provider questions or direct them to where they can go for help.
What has changed for me?
AAAs partner with the Next Generation MyCare plans to support members in getting the care they need by acting as waiver service and/or care coordinators. The plan’s delegation model determines how you work together to serve members.
- Full Delegation: AAAs serve as a member’s waiver service and care coordinator.
- Partial Delegation: AAAs or the Next Generation MyCare plan may serve as a member’s waiver service coordinator or care coordinator.
What has changed for members and where can they get help?
Eligible members are now receiving benefits through a Next Generation MyCare plan. Members have enhanced benefits including a care team, better transportation options, more in-home providers, and shorter wait times for prior authorizations.
Individuals who are eligible for the program and were previously enrolled in an Ohio Home Care, Assisted Living, or PASSPORT waiver program are now enrolled in the MyCare Ohio waiver. In the wavier program, they have the same benefits, or more, available to them.
If members have questions related to eligibility, enrollment, benefits, plan selection, or finding a doctor, they can contact the Ohio Medicaid Consumer Hotline at 800-324-8680 or https://ohiomh.com/. Representatives are available Monday through Friday 7 a.m. – 8 p.m. and Saturdays 8 a.m. – 5 p.m. Eastern time.
What has changed for providers and where can they get help?
In the Next Generation MyCare program, providers must enroll with ODM and contract with the Next Generation MyCare plans to provide services to members. Additionally, the way they submit Electronic Data Interchange (EDI) claims for MyCare members has changed. EDI claims will now come through the Ohio Medicaid Enterprise System (OMES) one front door.
If providers have questions related to OMES submitted claims, prior authorizations, member eligibility, provider contracting, waiver support, or general Medicaid billing they can contact the ODM Integrated Helpdesk at 800-686-1516 or IHD@medicaid.ohio.gov. Representatives are available Monday through Friday, 8 a.m. - 4:30 p.m. Eastern Time.
Where can I learn more about the Next Generation MyCare program?
Again, thank you for your commitment as we work to roll out the Next Generation MyCare program across the state.
|