
|
ODM Press
January 1, 2026
The ODM Press is a periodic email update on the progress of the ODM strategic initiatives for providers, associations, and advocacy organizations.
|
|
|
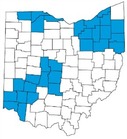
The Ohio Department of Medicaid (ODM) is dedicated to helping providers deliver the highest quality care to meet the healthcare needs of members. That’s why we are rolling out the Next Generation MyCare program, an improved healthcare program for Ohioans who have both Medicaid and Medicare. The program is now available in 29 counties across the state. Later in 2026, the program will be available in the rest of Ohio. |
|
 |

In the Next Generation MyCare program, providers must enroll with ODM and contract with the Next Generation MyCare plans to provide services to members. Ohio Department of Aging (AGE) enrolled providers can continue to provide services and submit claims but must contract with the Next Generation MyCare plans if you have not already.
If you have members who are changing plans or newly enrolled in the program, you can continue to provide services for a certain amount of time without having a contract with the Next Generation MyCare plans. If you want to continue to serve members in the program past the transition period, you need to contract with the plans.
|

The process for submitting Electronic Data Interchange (EDI) claims in the Next Generation MyCare program has changed. If you are not an Ohio Medicaid provider, your claims will be rejected.
-
If you are submitting your claims to the plans portal using Direct Data Entry (DDE), submit a single claim to the plan via their existing process. The plans do not accept paper claims.
-
If you are submitting an EDI claim for a dual benefit member or for a Medicaid-only member where Medicaid is the primary payer, submit the claim through the one front door, to the Ohio Medicaid Enterprise System (OMES). You must use the member’s Medicaid ID number. The submitted file must use the Next Generation MyCare Plan Receiver ID and the appropriate Payer ID in the 2010BB loop for claims to be directed to the correct plan for processing.
-
If you are submitting an EDI claim for a Medicare covered service for a Medicaid-only member, submit the claim to the primary payer.
-
If Medicare is the primary payer, submit the claim to Medicare using your normal process. Claims for Next Generation MyCare members will be automatically crossed-over to the plan.
-
If the primary payer is a Medicare Advantage/Part C plan, submit the claim to that payer using your normal process. Once the primary payer has adjudicated the claim and returned the Remittance Advice, submit the claim through the OMES one front door as described for a dual benefit claim.
Claim submissions through the OMES one front door are based on the date of submission. Any claims submitted starting today, January 1, 2026, should be submitted to the OMES one front door, even if the date of service was before January 1, 2026.
Aetna Better Health of Ohio and United Healthcare Community Plan are no longer MyCare plans as of December 31, 2025, however, they will continue to pay claims for up to 365 days from the end of the year and are responsible for any claims that have dates of service through December 31, 2025. Any claims should be submitted to Aetna or United using existing processes.
|

Ensuring members receive care is ODM’s priority. To verify if an individual is enrolled in a Next Generation MyCare plan, you can take the following actions:
- Check the Member ID Card. If the ID card has a Next Generation MyCare program logo, it is indicative that the member is a Next Generation MyCare member.
- Check member eligibility via Provider Network Management (PNM) or the EDI 270/271 process.
If after completing these steps you encounter issues verifying a member’s enrollment, we encourage you to provide the member services and follow existing billing guidance. If you have questions or need help, call the ODM Integrated Helpdesk at 800-686-1516 or IHD@medicaid.ohio.gov. Representatives are available Monday through Friday, 8 a.m. – 4:30 p.m. Eastern Time.
|

If you have questions about claims, prior authorizations, contracting, or other provider-specific functions, we are here to help. Contact ODM Integrated Helpdesk at 800-686-1516 or IHD@medicaid.ohio.gov from Monday through Friday, 8 a.m. – 4:30 p.m. Eastern Time. If you have questions about a Next Generation MyCare member’s Long Term Care Services or waiver service status, call the member’s plan or call the ODM Integrated Helpdesk. You can also view the Next Generation MyCare Provider Help Desk One-Pager to learn more about the additional help desks available to you.
|
Return to Top

Today, eligible individuals living in one of the 29 counties where the program is available started receiving care through a Next Generation MyCare plan. A dual benefit member gets their Medicaid and Medicare benefits from their Next Generation MyCare plan, and a Medicaid-only member gets only their Medicaid benefits from their Next Generation MyCare plan.
Members who were in the Ohio Home Care, Assisted Living, or PASSPORT Waiver when they were enrolled in the Next Generation MyCare program are now enrolled in the MyCare Ohio Waiver. In the MyCare Ohio wavier program, they have the same benefits, or more, available to them.
Members should have received a Next Generation MyCare member ID card in the mail to use at their appointments with you. If a member did not receive their ID card, needs to replace it, or their information needs to be updated, they should contact their plan. If they do not know their plan or have questions, they should contact the Ohio Medicaid Consumer Hotline at 800-324-8680. Check out our Next Generation MyCare Member ID Card One-Pager to learn more.
For members who experience a change in plans as part of the Next Generation MyCare program implementation, their Next Generation MyCare plan allows them to receive pre-authorized services and keep their current doctor for a period of time. After that period, members must use doctors who are in their plan’s network.
How can you support members?
If a member has questions about their Next Generation MyCare plan or benefits, direct them to contact the Ohio Medicaid Consumer Hotline at 800-324-8680 Monday through Friday 7 a.m. – 8 p.m. and Saturdays 8 a.m. – 5 p.m. Eastern time or visit www.ohiomh.com.
|
Return to Top
ODM is revamping the ways we connect with providers and all our members. Follow us for updates on healthcare coverage, wellness tips, and important information for Ohioans. Stay connected and informed about the latest initiatives and resources available.
 Return to Top
|
|
Feel free to distribute the information contained within this update to your colleagues, organization's members, or with anyone who you think might find it useful. We want all Ohioans to know what is going on with ODM's strategic initiatives.
Please also encourage anyone who you think might be interested in receiving similar updates to subscribe to the ODM Press. To view our past newsletters, please visit our website here.
|
|
Connect with us
|
|
If you wish to stop receiving messages from The ODM Press, you can update your preferences or unsubscribe from this list.
|
|
|
|