|
On March 22, Hennepin Health was featured in The New York
Times for its innovative health care reform efforts! Read the article here.
Back to top
 Hennepin
County Medical Center has embedded two Hennepin Health-funded community
paramedics at Harbor Light Center at 1010 Currie Avenue.
The paramedics are there on Sunday, Monday, Tuesday, and Friday from 4:30 p.m.
to 1:30 a.m.
Harbor Light Center is Minnesota’s largest adult outreach
facility, and the days and times the paramedics work there correspond with the
facility’s peak concentration of 911 calls — which increased 21.8 percent
between 2010 and 2014. They’re also periods when Harbor Light Center’s Health Care for the Homeless clinic is
closed.
Through this initiative, Hennepin County Medical Center aims
to reduce total cost of care by 10 percent — by avoiding unnecessary ambulance
runs and emergency department admissions and by linking residents to primary
care. On the first day, the paramedics triaged and cared for 11 residents; only
two were in true need of emergency department intervention.
In Minnesota, community paramedics can now bill Medical
Assistance (Medicaid) for some services. However, this type of staffing is possible only through flexible payment
models like Hennepin Health’s.
Kristopher Ehlert and Dennis Combs, the two paramedics
assigned to this project, have focused on building relationships with
residents, security guards, and homeless advocates. Instead of calling 911, “Call
or come find us,” they explain.
 Initially, it was chaotic. “An ambulance would arrive that we hadn’t called,” said Ehlert. “It took a few nights to change people’s thinking.”
But he’s seen signs that relationships are forming and ambulance calls are being prevented. The day we visited, as Ehlert approached the center a few minutes before 4:30 p.m., a resident who was standing outside greeted him with an enthusiastic, “Hi Kris!” And at 4:30 on the dot, he received a phone call from one of the homeless advocates about a member to check on.
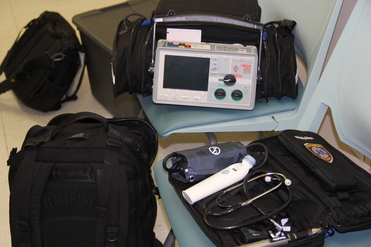
The project represents a new way of work for community
paramedics. One paramedic typically roves the facility while the other is
stationed in the Health Care for the Homeless clinic. Each paramedic carries a
cell phone with a number that they’ve given to staff.
 The paramedics’ interactions are often primary-care focused,
laced with conversations about medication management, diet, and setting up
outpatient appointments. The interactions also last longer. “On an ambulance I
would have spent five minutes with a person,” said Ehlert. “I spent 40 minutes
with a person today.”
Ehlert described an asthmatic resident who was recently
discharged from the hospital and wheezing. “Normally, someone would have called
911 about him,” said Ehlert. “Instead they called me.“ Ehlert showed the man
how to properly use his nebulizer and inhaler. After a few minutes, his
wheezing subsided.
Back to top
NorthPoint Health and Wellness Clinic is
piloting a project that may help with the state’s shortage of psychiatrists.
The Hennepin Health reinvestment initiative funds a
part-time psychiatrist who consults with primary care physicians and a psychiatric
nurse about patients’ medications.
The aim is to make primary care physicians more comfortable
with caring for — and prescribing medications to — patients with psychiatric
needs. Of Minnesota’s 87 counties, 74 don’t have enough mental health practitioners,
according to the U.S. Department of Health and Human Services.
 Psychiatric nurse Sophia Williams-Ogu was hired through the
initiative. Twice a week Williams-Ogu consults with psychiatrist Israel Sokeye,
M.D., about a panel of patients — one hour on the phone and one hour in person.
Then she routes Sokeye’s recommendations — such as starting, stopping, decreasing
or increasing a patient’s medications — to physicians. Sokeye is also available
to talk to physicians for 30 minutes four times a week.
Since the project launched, Williams-Ogu and Sokeye have
attended to the needs of nine Hennepin Health members. The goal is 75 members
over nine months. Williams-Ogu believes the goal is feasible; “We anticipated a
ramp-up period,” she said.
She’s started to receive referrals from Cerenity Petracek, a Hennepin Health-funded social
worker in Hennepin County Medical Center’s Acute Psychiatric Services. Other patients
with psychiatric needs have been identified through NorthPoint’s group visits and through Epic,
Hennepin Health’s electronic health record. NorthPoint recently hired a
community health worker who will locate patients for the project.
Psychiatric medication management is not the only need
addressed. Williams-Ogu connects patients to food, housing, transportation, chemical
dependency services, a health care home and more. “You need to look at the
whole person. Everything matters,” she said.
Williams-Ogu has been a psychiatric nurse for 16 years. She
has worked in inpatient and outpatient settings with children, adults, seniors,
and people with learning disabilities.
“I’m drawn to the challenge of keeping people out of crisis
care,” she explained. “I’ve seen that psychiatric medications can work.”
Later this year, Hennepin Health will evaluate the project
on a number of metrics, including change in patients’ emergency department
utilization, inpatient hospitalization utilization, and self-reported scores on
behavioral health questionnaires.
Back to top
Hennepin Health has committed to working with its providers to implement trauma informed care principles at its sites. Each month, the newsletter will feature a trauma
informed care domain, including practical implementation tips and work within the system that represents this domain.
 Domain #1:
Screening and Assessment
Trauma informed care is a shift in the way we work with people. Even
small steps can lead to big change. It may be helpful to approach the task of
screening and assessment with this in mind.
When and how do you ask about trauma? What do you do when the person
you’re meeting with actually talks about their trauma?
Even experienced mental health professionals struggle with asking
specific questions and fear triggering or re-traumatizing their clients. Yet,
trauma screening and assessment is crucial.
What we
know about screening and assessment:
1.
The ACES study tells us that we are missing
important health information if we don’t know about the traumatic experiences
of the people we work with.
2.
If we don’t ask, the people we work with won’t
necessarily tell us about their traumatic experiences.
3.
It’s important to ask about specific traumatic experiences. For example asking, “Have you
experienced trauma?” will not yield the same response as asking a patient “Have
you ever been physically injured by someone you love?”
Screening can range from a simple conversation and asking specific
questions to using standardized assessments. For example, in their article “Identifying,
Treating and Referring Traumatized Children: the role of pediatric providers,” Cohen,
Kelleher and Mannarino recommend that pediatricians simply ask at every visit:
“Since the last time I saw your child has anything really scary or upsetting
happened to your child or anyone in your family?”
The way to
ask (and what to do with the answer)
Often, the way providers ask the question is more essential than the
actual question.
Think about how you respond to the question, “How are you?” Your
response likely depends on how you’re asked. Was it an off-hand remark or did
the asker sit down, make eye contact, and express genuine interest?
It’s the same in our practice. When asking about trauma, always
present a calm, present, unhurried demeanor. Be genuine and act interested.
Many providers are afraid to ask about trauma. They fear they won’t
know what to do with the response and don’t want to cause more harm. The thing
to remember is this: People who have experienced trauma live with those
memories every day. When we ask about these experiences, we validate the
immense impact these experiences have on their lives. We send the message that
those experiences matter and can impact their health.
When trauma is disclosed, the most important response is validation
and sincere acknowledgment of their experience, not avoidance. Having a couple
of simple phrases in mind such as, “I’m sorry that happened to you,” or “No one
should have to go through that,” stated in an unhurried, caring way, can make
it easier to ask the questions.
After disclosure and validation of trauma, follow up with questions
such as, “Do you think these experiences impact your health?” or, “We know
there is a link between these types of experiences and a person’s health; have
you had a chance to explore this?” These help to focus the conversation, lead
to further education about the impact of stress on health, and open up the
opportunity to gather more information that will help providers treat the
entire person, rather than just physical illness.
If a person who discloses trauma asks for help in dealing with their
experiences, have trauma-focused therapy referrals ready, just as you might
refer to a specialist for other health concerns.
Within
Hennepin Health — a poster opens the conversation
Heidi
Carlson, clinic supervisor for Hennepin County Healthcare for the Homeless,
noticed a patient looking closely at a poster on the wall of the clinic at
Harbor Light Center. The poster described adverse childhood experiences and
their impact on health.
 Heidi
asked the patient if she could relate to the experiences on the poster. The
patient looked up and replied, “I’ve had all of them.”
Heidi
then asked if she had experienced any of the health effects listed on the
poster. The patient pointed out several, but after a self-reflective pause
remarked, “But I’m still here, aren’t I?”
Heidi
was surprised at how easy it was to talk about trauma and was struck by the
depth of conversation spurred by such a small intervention — the poster she got
from a trauma informed care training and put on the wall.
Resources
This article was published recently through national public radio and
addresses this topic:
http://www.npr.org/blogs/health/2015/03/03/377569539/even-some-doctors-fear-these-10-questions
The American Academy of Pediatrics developed a
guide for addressing trauma in primary care:
https://www.aap.org/en-us/advocacy-and-policy/aap-health-initiatives/healthy-foster-care-america/Pages/Trauma-Guide.aspx
Back to top
|