COVID-19 Alaska Clinical Update, Aug. 1
Alaska DOH sent this bulletin at 08/01/2020 11:29 AM AKDT
Cumulative Cases
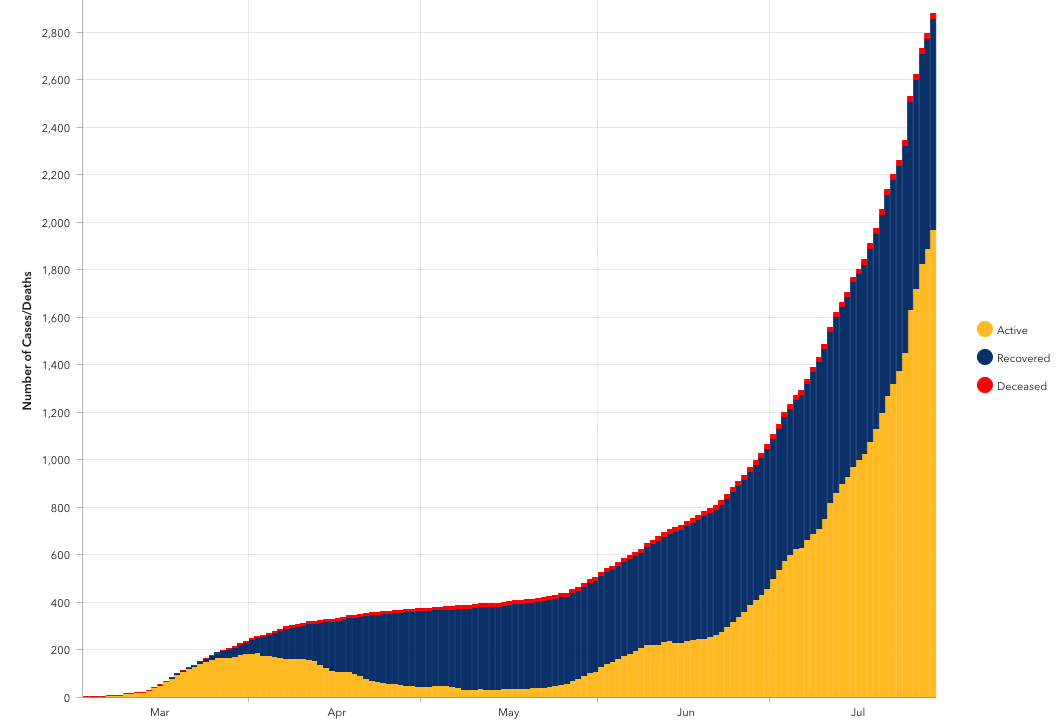
|
Even young, healthy adults may have symptoms for weeks
292 US adults who tested positive for SARS-CoV-2 at an outpatient visit were interviewed via telephone 14-21 days after the test date. 94% reported experiencing symptoms at the time of testing, and 35% of these reported not having returned to their usual state of health by a median of 16 days from their testing date. This included 26% of 18-34 year olds, 32% of 35-49 year olds, and 47% among those aged 50 or older. 43% had a lingering cough, while 35% reported ongoing fatigue and 29% persistent shortness of breath. People reporting two or more chronic medical conditions were also more likely to report having not returned to their usual state of health within 2-3 weeks; 28% of those with no or one chronic medical condition compared to 46% with two and 57% with three. 19% of adults aged 18-34 years who reported no chronic medical conditions had not yet returned to their usual state of health at 2-3 weeks after their positive test. MMWR authors conclude that COVID-19 can result in prolonged illness even among persons with milder outpatient illness, including young adults and those without chronic illnesses. While news media has focused on the significant risk of severe COVID-19 in people aged 65 or older and those with chronic medical conditions, clinicians can help educate patients and communities that COVID-19 can cause severe illness at any age and may cause unpleasant symptoms lasting weeks even in young, healthy adults with mild cases. As cases in Alaska have risen most sharply among adults aged 20-39 in recent weeks, there is increased urgency to help younger adults appreciate the importance of physical distancing, wearing face coverings, socializing within a household bubble, and taking other actions to reduce the spread of COVID-19.
Remdesivir, reviewed
A review in Infectious Diseases and Therapy considered all available evidence regarding remdesivir for COVID-19 through the end of May. In patients admitted to the hospital not requiring supplemental oxygen, there may have been a modest benefit in time to clinical improvement but not a difference found in progression of severity of disease or death, likely because of the low incidence rate of these in this patient group. A clinically meaningful benefit was seen in patients requiring low-flow supplemental oxygen, both in mortality and decreased time to recovery, in two major trials, with the caveat that one small RCT failed to show a difference. Patients needing high flow oxygen or noninvasive ventilation had mixed results that authors conclude do not support a clinically meaningful benefit in this patient group; while patients requiring invasive mechanical ventilation were not found to receive benefit from remdesivir.
Mitigation in Milwaukee
Wisconsin held a statewide primary election fewer than two weeks after a stay-at-home order was issued, implementing CDC polling location guidance including tape-marked increments in lines, voting booth spacing and metering, encouraging mask wearing, cleaning high-touch surfaces, PPE and training for poll workers, encouragement of absentee voting and scale-up of curbside voting. No clear increase in cases, hospitalizations or deaths was observed in an election when more than 18 thousand people voted at just five in-person polling places, suggesting possible benefit of the mitigation strategies in preventing SARS-CoV-2 transmission. Absentee mail-in ballots were used by nearly 65,000 voters, while another nearly 12,000 voted early or curbside; 176 of 181 previous polling sites remained closed. However, compared to a similar election in spring 2016, the total number of people voting decreased 43%.
SARS-CoV-2 pediatric viral load
A letter in JAMA Pediatrics this week reported an analysis of the nasopharyngeal viral nucleic acid amount in 145 patients testing positive for COVID-19 in Chicago, grouping them by age. Amount of nucleic acid present was estimated by using the PCR amplification cycle threshold value for a given nasopharyngeal swab, with lower cycle threshold (CT) values indicating higher amounts of viral nucleic acid (i.e. fewer PCR cycles were needed to amplify the nucleic acid present in order to reach the detectable threshold). Patients with severe infection were excluded as they are known to have higher viral nucleic acid amounts, so 7 children requiring supplemental oxygen were excluded. Asymptomatic patients were also excluded, as were those with symptoms for more than 1 week prior to testing or unknown duration of symptoms. The cohort of 46 children under age 5 was compared to a cohort of 51 children aged 5 to 17 years and 48 adults aged 18 to 65. While the latter cohorts were similar at CT values of 11.1 [IQR 6.3-15.7] and 11.0 [6.9-17.5] respectively, the youngest cohort had median CT values of 6.5 [4.8-12.0], corresponding to approximately 10x to 100x greater viral nucleic acid isolated from an NP swab in the youngest cohort. Authors conclude that this indicates that there were ‘significantly greater amounts of viral nucleic acid detected in young children’ and ‘young children have equivalent or more viral nucleic acid in their upper respiratory tract compared with older children and adults’.
While the medians in this study do differ between cohorts of children under 5 and older children or adults, there are several limitations to then directly drawing a conclusion that young children with COVID-19 are significantly more infectious or, indeed, have more viral nucleic acid in their upper respiratory tract. One alternative explanation might be that a higher viral load is needed for children under 5 to have symptoms with COVID-19; this study excluded asymptomatic positive cases. Additionally, while the abstract states young children had significantly greater amounts of RNA detected, the overlapping interquartile ranges of their data do not support statistical significance, which is likely why authors qualified their results section by stating that ‘young children have equivalent or more viral nucleic acid… compared with older children and adults’. While a small Swiss study isolated infectious virus from symptomatic children of all ages in early acute COVID-19, it is impossible to say on the basis of the Chicago data whether young children with COVID-19 are more, less, or equally infectious as older children or adults.
|
