COVID-19 Alaska Daily Clinical Update, June 1
Alaska DOH sent this bulletin at 06/01/2020 07:35 PM AKDT
Monday, June 1, 2020
Liz Conway Ohlsen, MD
With information from Anne Zink, MD, FACEP, Alaska Chief Medical Officer
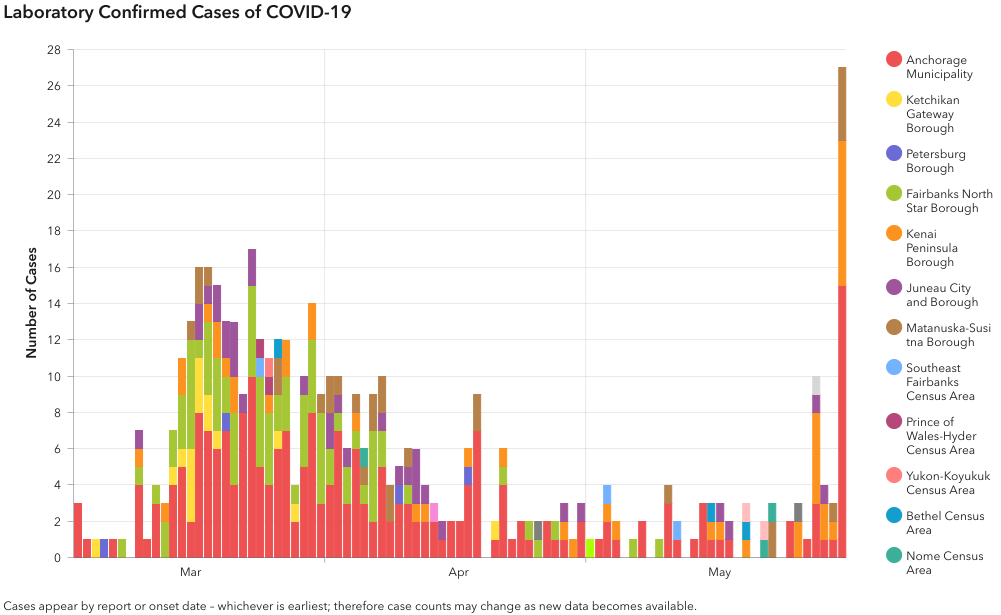
Alaska saw its largest single day increase in cases yesterday
Twenty-seven cases were identified yesterday. Among them are 12 new cases in Anchorage, 3 in Eagle River, 4 in Wasilla, 3 in Kenai, 1 in Soldotna, 1 in Anchor Point, 1 in Homer and 1 in Kenai Peninsula Borough. Nine of the twenty-seven are aged 60 or older, while four are under age 20. The nonresident total also increased by 1 after a case was found in a seafood worker in Dillingham, for a total of 21 recognized in nonresidents and 460 in Alaska residents. These cases join others in a four-day run late the week after Memorial Day; there have been 44 cases over the last 4 days. 20 of those have been in the Anchorage borough, 5 in Mat-Su, 16 on the Kenai Peninsula, two in Juneau and one in North Slope Borough.
Cases are linked to a skilled nursing facility and large gatherings
10 of the cases identified yesterday are among patients and caregivers at a skilled nursing facility in Anchorage, joining two previously identified active cases among patients at the same facility. Additionally, some of the cases reported yesterday were linked to large gatherings on the Kenai Peninsula, reinforcing the need to counsel our patients to avoid large groups and that anyone with symptoms must stay home.
Nursing home guidance
Skilled nursing facilities, long term care facilities and adult living facilities house medically vulnerable people in a congregate setting and are at high risk from COVID-19. One of the earliest US clusters of COVID-19 was in a nursing home in Washington State, in which 58 of 90 residents tested positive. Alaska has previously had a cluster of COVID-19 cases associated with a skilled nursing facility in Fairbanks, involving three residents and multiple staff members.
CDC provides guidance for nursing homes that covers management, infection control and preventing transmission between residents and caregivers. In terms of management, they recommend each facility have someone with training in infection prevention and control manage on-site prevention and response, report COVID-19 cases and staffing to a centralized system weekly and have a plan for COVID-19 testing, cohorting and managing admissions. Management should also ensure adequate PPE availability, including planning ahead for a possible outbreak in the facility. For infection control among residents and their families or other visitors, facilities must regularly monitor patients for symptoms and implement precautions immediately on suspecting COVID-19. They should educate residents, caregivers and visitors about COVID-19 precautions and prevention, implement source control measures including enforcing respiratory hygiene and cough etiquette, having hand sanitizer readily available, and having all residents wear cloth face coverings whenever possible, and restrict visitors as much as the local situation requires. In terms of preventing transmission between patients and caregivers, caregivers should wear facemasks when around residents (not just cloth face coverings). All healthcare workers should be screened for fever and other symptoms at the beginning of each shift. Facilities should institute a system for sick leave that is flexible and not punitive for caregivers and encourage them to stay home when ill. They should also restrict all non-essential healthcare personnel and implement telehealth where possible.
In facilities that need to cohort residents and establish a designated COVID-19 care unit, further guidance is available.
CMS has made some accommodations to support facilities in adjusting to changes related to COVID-19.
US and global update
US known cases are more than 1.8 million, with more than 104,000 reported deaths. Worldwide, more than 6 million cases have been diagnosed, with more than 370,000 confirmed deaths, about 6%.
|
