The SEGIP Report - An Employee Newsletter - Volume 9, Issue 1 - March 2016
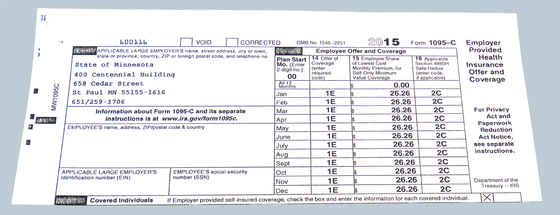
IRS Form 1095-C – It’s in the mail
Check your mailbox! We recently mailed an IRS Form 1095-C to
participants in the state’s employee health plan. If you got one, you may be
asking what to do with it.
The Form 1095-C is the W-2 of health insurance. It provides
information about your employer’s offer of health insurance coverage and the
months in which you and, if applicable, your dependents, had coverage.
Unlike the W-2, you do not include your 1095-C (or 1095-B) with
your tax return. Keep it with your other important tax documents.
Employers are required to send the IRS a copy of each 1095 they
gave their employees. The IRS will use these forms to identify the months enrollees
had coverage.
SEGIP sent a 1095 to any employee/policy holder who during any
month of 2015:
-
Received coverage through SEGIP, or
-
Was a retiree under the age of 65 or other non-employee
who received coverage through the state (even if you paid your premium to one
of the three plan administrators including Blue Cross Blue Shield, HealthPartners,
or PreferredOne).
Retirees over age 65 will not receive a form because the
coverage received through the state is not primary coverage.
We did not send a separate form to anyone else on your
coverage, including an adult child, your spouse, or former spouse. Please
provide a copy to those who may need it.
For more information:
-
Check with the IRS
- See the FAQs on the SEGIP website
-
Call SEGIP at 651-355-0100

NEW! Diabetes MTM program now available to dependents
The Diabetes Medication Therapy Management (MTM) program provides
health improvement and financial benefits. We expanded the program to include dependents
with diabetes who are over the age of 18.
Now both employees and dependents enrolled in the Minnesota
Advantage Health Plan have additional support to manage their condition.
- Dependents can visit the MTM Dependent
Program page for more information. Their
copays are waived on formulary diabetic supplies and medications.
-
Employees
with diabetes not previously enrolled can start now. Visit the MTM Employee Program page for more details. The program encourages and rewards lifestyle changes.
The MTM program is a great way to help keep your
diabetes in check while protecting your pocketbook.
|
MDEA shopping made
easy
Check out the FSA
Store. It is a website that only
sells FSA-eligible items (some require a doctor’s prescription prior to
purchase and are noted on the site). Use
the Benny Card to pay for your items and avoid the need to save receipts. Use this coupon to make
shopping even easier (one per customer).
 Check your
mail – it’s to your advantage
Multiple
times a year, SEGIP sends out important communications through the postal
service. Some of our letters and packets give you 30 days to reply with a
document or a payment. Late submissions or payments can result in the loss of
your coverage. Please open your mail on a timely basis.
Keeping
your mailing address up-to-date in Self Service is also extremely important, as
that’s the only way we can reach you with these vital forms
|

Benny needs your help – to prove it
The Benny Card does not eliminate the IRS requirement to verify
that all expenses are eligible. Benny is not always able to determine this
automatically.
Helpful things to know about
Benny:
- 87% of Benny Card charges are automatically
approved without a request for documentation.
- Most prescription copays and medical charges are approved
at the point of service because they either match the Benefits Schedule
copayments or match through a transaction match system.
- Dental and vision charges often require
documentation because the costs vary and these providers can offer ineligible
services such as cosmetic treatments and product warranties.
-
For charges not automatically approved,
you will be asked for documentation of the charge. Due to the system’s attempts at auto-matching
a transaction, this request may happen a month or two after the date of the
transaction.
Here’s how you can help:
- Keep your receipts so that you can provide
documentation when requested by 121 Benefits.
- Don’t ignore the requests for documentation.
-
Know that a request for documentation does not
necessarily mean the charge is ineligible. It means that Benny is not able to
determine if the charge is eligible.
- Submit documentation on time. Benny will be
temporarily suspended if documentation is late and will remain inactive until
documentation or repayment is provided.
-
Not submitting documentation will be considered
an overpayment from your account and the amount will either be deducted from your
state tax refund or included as taxable income on your W-2 form.
It’s easy to submit documentation. You can do it online,
or via the U.S. mail, fax, or smart phone.
Find more information on debit card transactions,
acceptable documentation, and the FSA Store on 121 Benefits’ website.
|

Healthy discounts
– just a click away with your insurance member ID card
Your medical and dental plan membership cards provide you
much more than clinic and co-pay information. They are also a pathway to saving. Find discounts on health and well-being products and services on your
plan’s website.
Examples of discounted
retail products and services beyond your medical and dental coverages:
-
Fitness and sport equipment
-
Exercise classes
-
Adult orthodontics
-
Food and nutritional counseling
- Eyewear
Not finding what you need online? Give your plan a call.
They’ll be happy to provide details about their member discount programs. These
discounts may change during the year, so be sure to check with your plan often.
Don’t have your member ID card handy? The SEGIP website has quick links to plans and
other resources.
|

Prevent – A whole new way to healthy
SEGIP will continue to offer the Prevent® health benefit a
breakthrough program that helps reduce your risk of developing type 2 diabetes. Prevent gives you the support
you’ll need to lose weight, keep it off, and make lasting lifestyle change.
Over 5,000 of your
colleagues are already onboard. They are seeing significant success at
reducing their risk for developing type 2 diabetes. Participants have lost over
16 tons!
The online program includes:
-
A health coach to keep you on track
- A wireless scale to monitor your progress
- An interactive program customized to you
-
Weekly online lessons that inspire
- Real-time
support
Get started today. Take a one-minute health test to find out
if you’re eligible.
This program is offered at no
cost to you!
|
| 









