 The Hennepin County Mental
Health Center is part of Hennepin County’s Human Services
and Public Health Department, one Hennepin Health’s four partner organizations.
Because of the high rate of mental health conditions in the Hennepin Health
population, the center plays an important role in the continuum of services
delivered to members.
The Mental Health Center provides
comprehensive outpatient mental health services to adults with serious mental
illness as well as those with co-occurring substance use disorders. The center also serves children and adolescents
with serious emotional disturbance.
Located on
the second and third floors of the Nicollet Exchange Building at 1801 Nicollet
Avenue, the Mental Health Center offers a range of services, including:
- Diagnostic assessments
- Psychiatric evaluations
- Psychological evaluations
- Individual and group therapy
- Medication management
- Dual-diagnosis programs (for co-occurring mental illness and substance
use disorders)
- Outreach to persons who are homeless
- Consultation
Sally Kratz and Amber Morgan
Sally Kratz, M.S.W., L.I.C.S.W,
administrative manager, and Amber Morgan, R.N., clinical care coordinator, are
two staff members at the center. Both play important roles in Hennepin Health.
 Morgan (left) with Kratz
Morgan joined the center in 2013
under a UCare grant.
When the grant expired in March 2014, Hennepin Health began funding Morgan’s
care coordination services via a 2014 reinvestment initiative.
Morgan's work appears to be having an effect. In late 2013, Dana Soderlund, M.P.H., Hennepin
Health data analyst, looked at the pre- and post-medical utilization rates of
56 Hennepin Health members who had received Morgan’s care coordination services.
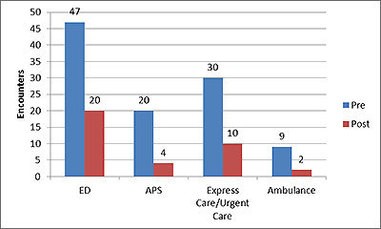
Soderlund determined that the total number of emergency department (ED), acute
psychiatric services (APS), urgent care, and ambulance encounters within the
cohort declined after Morgan’s engagement. This chart depicts the decline:
 Kratz, who has worked at the Mental Health Center since 1999, has seen the
benefits of Hennepin Health’s integrated care model. As a long-time clinician treating persons
with severe psychiatric disorders, she believes that traditional models of care
have been inadequate and unresponsive to the many and varied client needs for
person-centered, individualized mental health services, primary and dental
care, and social services. For Kratz, having the opportunity to participate in the planning and
implementation of care coordination at the Mental Health Center has been both challenging and
rewarding.
The center hopes to build on the success of care coordination
services and further develop and sustain innovative approaches to service
delivery.
Charles
One Mental Health Center patient is 46-year-old Charles, a Hennepin Health member who was incarcerated for 26 years (from age 18 to 44) in Saint Louis, Missouri. Although Charles doesn’t excuse the actions that led to his incarceration, he notes that his early life experiences — including a physically abusive stepfather — informed some of his choices.
 Before,
during, and after his release, Charles struggled with a host of mental health
and chemical dependency issues including depression, anxiety, antisocial
personality disorder, post-traumatic stress disorder, and alcoholism. The experience prompted him to
relocate to Minneapolis in 2012; Charles believes that Minnesota’s behavioral
health infrastructure is superior to many states.
From August 2012 to March 2013,
Charles lived at House of Charity
in Minneapolis. Here, an advocate connected him with Hennepin Health and the
Hennepin County Mental Health Center.
Since he started visiting the Mental Health Center, Charles has interacted with a range of behavioral health providers,
including Dr. Ngozi Wamuo, a psychiatrist; Mary Shannon-Myer, a therapist; and
Amber Morgan. First, he began taking medications to help manage his symptoms and
worked with Shannon-Myer to identify and address obstacles to progress. Then Shannon-Myer introduced Charles to Morgan for care coordination.
Morgan helps Charles set up his
medical and dental appointments. She is also a skilled listener, someone Charles
can talk to “without being judged.” Morgan introduced Charles to Connections —
a men’s treatment group that meets on Tuesdays and Fridays — that she helps
facilitate.
Initially, Charles was
resistant to Connections because he was uncomfortable with sharing his story in
a group. Once he started attending, however, Amber and the members won him over
with their lack of judgment. Today, he
credits this willingness to share his feelings and experiences — instead of
bottling them up — as key to his recovery.
 One of Charles’ most memorable
moments in Connections occurred during his second meeting, when a man in the
group — who, Charles says, bore a striking resemblance to his biological father
— told Charles that, “The greatest thing a person in our position can do” is be
compliant with their medications. At the time, Charles did not take his
medications consistently — in part, because he worried about their side
effects. However, the man’s statement inspired Charles to “create a regimen”
around taking his six prescriptions.
Charles has also found the
Mental Health Center's weekly Mental Illness Chemical Dependency (MICD) treatment group helpful.
A person with long-time alcohol dependence, Charles traces his substance abuse
to his stepfather; after being physically abused, he explains that he began to
use alcohol as a way to “abuse myself,” and as a coping mechanism
One Thursday in February 2014,
Charles was on the number 18 bus, enroute to the MICD treatment group, when he
had a moment of weakness. He explains that he rode past the center and got off
downtown at Nicollet Mall. He bought a pack of cigarettes at a drug store, and
was about to buy alcohol next, when he had a moment of clarity and remembers
thinking, “The liquor store has nothing to do with my life right now.”
He got back on the bus and returned
to the Mental Health Center.
Today, Charles describes
himself as “stable” and mostly sober, but still prone to occasional bouts of depression,
anxiety, and post-traumatic stress disorder. He believes that one of his greatest accomplishments is the
confidence he’s gained in his ability to follow through. Kratz calls this confidence
“emotional muscle.” Charles identifies it as the thing that prompted him to get
back on the bus and return to the Mental Health Center, the thing that compels him to take his
medications each day.
A few months ago, St.
Stephen’s Human Services invited
Charles to speak to a group of women about his life story. Charles was well
received, and the experience made him realize that opening up could be
beneficial not only to himself, but to others. “I have a lot to give,” he
notes. “If [sharing my story] could deter one young man from getting in trouble
or going to prison, then I’ve succeeded.”
On May 1, Charles accomplished
one of his goals — he moved into his own apartment, a one-bedroom near Lake
Calhoun that staff at St. Stephen’s helped him find. Other goals include
remaining sober, banishing negativity, and continuing to learn how to “function
in society.” Charles believes that it’s important to set realistic goals and to
take things a step at a time.
“I can’t think about the future
until I think about today,” he says.
Looking ahead
Kratz and Morgan are optimistic
about the future of behavioral health care in Minnesota. Here are four trends
they’ve noticed:
- Increased
recognition of psychiatric illness as a public health issue; it affects more
than the individual
- Increased
acknowledgement that integrating medical, mental health, and social needs is
effective
- Increased
recognition that poverty is a barrier; it’s difficult to focus on recovery when
you’re thinking about survival and basic needs
- Less
stigma attached to mental health issues
Mental Health Center location,
contact information, and hours
Nicollet
Exchange Building
1801 Nicollet
Avenue
2nd
and 3rd floors
Minneapolis,
MN 55403
General information:
612-596-9438
Appointments:
612-596-9438
Fax:
612-879-3824
Monday,
Tuesday, Thursday, and Friday: 8 a.m. to 5 p.m.
Wednesday: 8
a.m. to 6 p.m.
Back to top
Judy Soderberg has been a member of Hennepin Health’s Care Model
Committee since 2012. While most of the committee is composed of employees from
Hennepin County Medical Center, NorthPoint Health and Wellness Center,
Metropolitan Health Plan, and Hennepin County’s Human Services and Public
Health Department — Hennepin Health’s four partners — Judy is retired and a
volunteer. One reason why she’s interested in Hennepin Health is because the
program provides health care for many people with behavioral health concerns.
Soderberg’s son Shean has paranoid schizophrenia.
 Shean, a few years after his diagnosis
Thanksgiving Day
“I call [Shean’s schizophrenia] ‘the journey,’” Soderberg said, over
coffee at a Dunn Brothers at Hennepin County Medical Center. “You don’t know
about mental illness, it may not be part of your knowing, unless it comes to
you in some way.” For Soderberg, that journey into knowing began on a Thanksgiving
Day about 25 years ago, when Shean was in his early twenties.
Soderberg recalled that because of their busy schedules she’d seen
Shean infrequently in the months leading up to that life-changing day. When he
arrived at her house on Thanksgiving, he appeared agitated and began pacing. He
then left abruptly — in Soderberg’s car — and didn’t tell anyone where he was
going.
When Shean returned a few hours later, Soderberg learned that he
had totaled her vehicle in Saint Louis Park.
Soderberg’s oldest son Aaron took Shean to Hennepin County
Medical Center. A string of hospitalizations followed. When Shean was diagnosed
with schizophrenia during one of these hospitalizations, Soderberg committed to
learning everything she could about mental illness.
Soderberg explained that a few months before that Thanksgiving
Day, Shean had been in a bicycle accident near Lake Calhoun and suffered a traumatic
brain injury. To this day, it’s unclear how much of Shean’s behavior can be
attributed to his traumatic brain injury versus his schizophrenia.
The aftermath
Soderberg noted that the years immediately following Shean’s
diagnosis were particularly difficult. Shean was hospitalized repeatedly,
including two hospitalizations at Anoka-Metro Regional Treatment Center for
almost two years each time. Between hospitalizations, he lived in different
places, including a group home and a board and lodge; for a while, he lived on
the streets. Because Shean didn’t want to accept that he had schizophrenia, he
resisted taking his prescriptions.
Soderberg believed that the turning point came when Shean was
able to come to peace with his diagnosis and, consequently, be compliant with
his medications.
Another turning point occurred when Soderberg, her ex-husband,
and their two other children — Aaron and Jennifer — came to a mutual
understanding that supporting Shean was “a family operation.” “The expectation
in our family is that everyone does something,” Soderberg said. She
characterized her role as Shean’s “unofficial case manager.”
Shean today
Today Shean lives in a supportive housing unit in Minneapolis.
He is a Medicaid recipient. He also qualified for a Brain Injury Waiver through the state
of Minnesota. The waiver covers a number of services, including an independent
living services (ILS) worker. Shean’s ILS worker visits him once per week to
help him with paperwork, grocery shopping, banking, and more.
 Shean today, with his daughter and grandson
Shean’s involvement in the Interact Center — which is also funded through the waiver — has
been particularly pivotal. Located in Minneapolis’ North Loop, Interact is a
visual and performing arts center for artists with disabilities. Shean, who is
in the performing arts track, typically spends three to five days per week at
the center. Soderberg said that Interact has given Shean a sense of purpose,
structure in his day, and new friends.
 The Interact Center is located at 212 3rd Avenue North #140
 Interact artists
Soderberg as an
advocate
Because of her personal experiences, Soderberg has become a
mental health advocate. “I look at myself as a reality check for people,”
she said about her involvement with Hennepin Health’s Care Model Committee.
One of the realities she is particularly passionate about sharing
is the state of transitional care (the health care a patient receives as they
move from one level of care to another, such as from a hospital to home).
Soderberg recalled an occasion when Shean struggled after his discharge from the
hospital because no one had helped him set up his medications.
Support
Do you have a family member or a friend with a mental illness? Here
are three resources that Soderberg recommended:
Back to top
In late 2012, Hennepin Health decided to use
a portion of its reinvestment initiative funds for a new county sobering center
at 1800 Chicago Avenue. The $185,000 allocation was to cover center start-up
costs, a van to transport patients, motivational interviewing training for
staff, and more.
Hennepin Health envisioned the new sobering
center as a 30-bed facility that could be used to divert chronic inebriates
from the emergency department to a lower — and less costly — level of care, if
clinically appropriate. A year later, despite having selected a preferred
vendor through a competitive proposal process, the sobering center is not yet
operational. Many people in the community are
wondering why.
Current status
In 2013, county officials reviewed the
space at 1800 Chicago Avenue. They determined that the facility needed several
upgrades in order to operate. It is estimated that these upgrades will cost up
to $4 million beyond the original $185,000. Further, the Minnesota Department
of Human Services (DHS) has indicated that the sobering center would need to be
licensed, but have not yet developed the licensing requirements. This has
pushed back the timeline for implementation.
Jennifer DeCubellis, assistant county
administrator, is scheduled to go before the Hennepin County Board of
Commissioners in June to present a business case for investing up to $4 million
in the sobering center. If approved, DeCubellis anticipates that it may
take about 18 months (November 2015) before the upgrades are made and the
facility is licensed. DeCubellis notes that there are other possible courses of
action, as well, such as finding an alternate facility that requires fewer
upgrades.
Currently, counties are 100 percent responsible for funding
their own detox services. However, due in part to the Affordable Care Act, the
national standard is expected to change. In the future, state and federal
Medicaid dollars will likely be another source of funding. At their June 2014
meeting, DeCubellis and the Board of Commissioners will discuss what entities
will pay for the sobering center and a timeline for when it will go
operational.
Policymakers have discussed a Hennepin County sobering
center for over 12 years. DeCubellis explains that this is an exciting time
because key stakeholders now support its creation, including the Minnesota
Department of Human Services and the local police department. As the year
progresses, Hennepin Health will continue to provide updates on this
reinvestment initiative.
Back to top
|