 Courtney describes 2010 as “the year my life fell apart.”
He got divorced. His mother died and so did a best friend and a coworker. The company he worked at encountered financial trouble and closed its doors. After a few months of unemployment, Courtney lost his car and apartment.
Initially, he managed his emotions by going out with friends for a beer. Soon, he was drinking more and more. His health deteriorated and he experienced insomnia and suicidal thoughts. He grew increasingly destructive — breaking windows and furniture — and eventually landed in jail.
Later, a nurse at the Hennepin County Adult Corrections Facility diagnosed Courtney with alcoholism and clinical depression and he began visiting the county’s Mental Health Center. Soon after, Courtney moved into Exodus Residence — a transitional housing facility in downtown Minneapolis — where, he says, staff “bent over backwards to help” and he began to formulate a plan to get his life in order.
When Courtney enrolled in Hennepin Health, he learned that it offers a myriad of medical, behavioral health, and social services. Courtney decided to capitalize on these diverse offerings, to “take any avenue I could take to get healthy.” For him, it was “do or die.”
Courtney started using Hennepin Health’s emergency department in reach program with RESOURCE Chemical and Mental Health. The program provides targeted case management for Hennepin Health members who are frequent users of the emergency department (to qualify, members must have visited the emergency department at HCMC at least three times in the past four months). The goal of the program is to increase these members’ access to preventative services while decreasing their reliance on costly emergency department and inpatient care.
RESOURCE Chemical and Mental Health staff work with Hennepin Health members for two to four months. They help members:
- Connect to social services like housing
- See a primary care provider
- Get medications
- Link to behavioral health and/or chemical dependency treatment
To find out more about this program or to refer a Hennepin Health Member, contact TJ Redig, RESOURCE Chemical and Mental Health team lead/case manager, at 612-750-5509 or tredig@resource-mn.org
Courtney says that Victoria Karpeh, one of RESOURCE’s emergency department in reach staff, has been invaluable to his recovery. In addition to day-to-day practicalities like reminding him to attend his medical appointments, Victoria listens to Courtney and encourages him to take positive steps. One of Victoria’s mantras has been particularly pivotal: “It’s going to be all right.”
Courtney lists off his short-term goals: find a stable job, pay his bills, remain sober, take his medications, and stay away from people who party.
He encourages Hennepin Health members — and others who are trying to turn their life around —to be proactive and take full advantage of the medical, behavioral health, and social service opportunities that are available to them.
 Renee Gust, M.A., R.N. is a senior health promotion specialist at Hennepin County’s human services and public health department where she teaches staff — at over 30 clinics in Hennepin County — techniques to improve the treatment of patients who have, or are at risk for developing, chronic conditions.
One of the techniques that Renee teaches is motivational interviewing, a form of health coaching that empowers individuals to take personal responsibility for their health.
Renee uses a motivational interviewing curriculum developed by Thomas Bodenheimer, a doctor at the University of California, San Francisco. Mainstays of Bodenheimer’s curriculum include:
- Ask-tell-ask: Using open-ended questions to discover what lifestyle changes a client is willing to make. This helps providers determine what advice is worth giving a patient (and what advice will likely go in one ear and out the other).
- Closing the loop: With teach-back techniques, a patient repeats the information they’ve been given. This ensures that the patient comprehends what they’ve just been taught.
- Setting the agenda: Prioritizing motivational interviewing techniques to avoid wasted time and visits.
- Medication reconciliation: Using methods to deal with medication non-compliance.
- Action planning: Helping patients set health goals and assessing a patient’s readiness to change.
Renee’s interest in prevention began early in her career. As an R.N. at HCMC, she worked to alleviate patients’ pain, but sometimes felt that the tools at her disposal—“medication and compassion”—weren’t enough, especially for those with chronic conditions. Saddened by the amount of suffering she saw, Renee increasingly desired to offer prevention tools instead of just “patching people up.”
This led her to the University of Minnesota, where she earned a master’s degree in liberal studies. The U of M’s MLS program is interdisciplinary. While Renee was interested in public health, she also wanted to infuse her studies with a business model and took project management courses at the Humphrey School of Public Affairs. After completing her degree, Renee transitioned from nursing to public health.
Renee is excited by the work she does with Hennepin County and believes that prevention is the future of health care.
According to Renee, motivational interviewing can help a patient with smoking cessation, weight management, physical activity, nutrition, medication adherence, chemical dependency, and more. In addition, a health coach who uses motivational interviewing can:
- Relieve the burden on doctors and nurses
- Empower patients to self-manage their health
- Save the system money by diverting patients from costly crisis care
Renee offers one-day courses on motivational interviewing. If you or your staff are interested in training or want to learn more, contact her at renee.gust@hennepin.us
 The Harbor Light Center at 1010 Currie Ave., Minneapolis, is Minnesota’s largest homeless adult outreach facility.
Hennepin County’s Health Care for the Homeless operates medical clinics at 11 shelters and drop-in centers in Minneapolis. These medical clinics are staffed by health care professionals who treat patients, prescribe medication, provide health care education, and link individuals to community resources.
Like NorthPoint Health and Wellness Center — one of Hennepin Health’s four partners — Health Care for the Homeless is a federally qualified health center. FQHCs receive grants under Section 330 of the Public Health Service Act and qualify for Medicare and Medicaid reimbursement. They provide primary care services to underserved areas or populations. FQHCs also offer a sliding-fee scale and serve people of all ages, regardless of an individual’s ability to pay or their health insurance status.
 Roosevelt, a Hennepin Health member, received a voucher to stay at Harbor Light Center. He currently lives in the shelter’s respite room, a 12-bed room for men with acute health care conditions. Roosevelt has a history of high blood pressure, heart attack, and mental illness. He receives care from the HCMC Whittier Clinic. He explains that Amber Altstadt, a pharmacy resident at HCMC, has been particularly instrumental in helping him manage his medications.
Who is eligible for Health Care for the Homeless in Hennepin County?
Any homeless adult or child living in situations such as:
- Outside or on the street
- In shelter or transitional housing
- With friends or relatives (“doubled-up” or “couch hopping”)
-
Currently housed but homeless within the last year.
How are clients referred to Health Care for the Homeless?
If you know a homeless individual who needs medical care:
- Have the person call 612-348-5553, or
-
Direct the person to a Health Care for the Homeless clinic
This brochure lists Health Care for the Homeless clinics in Hennepin County.
 Nancy Liddy, N.P., says that she treats homeless patients for chronic conditions (e.g. diabetes, high blood pressure, mental illness, chemical dependency), as well as for “simple things” like colds that most of us would never worry about paying for. Nancy often encounters foot problems like blisters, callouses, and athletes foot in her homeless patients. “They do a lot of walking in bad shoes,” she explains.
The Hennepin Health connection
Stephanie Abel, Health Care for the Homeless clinic manager, has been a member of Hennepin Health’s care model committee since 2012. Through her involvement with Hennepin Health, Stephanie has made connections with people across Hennepin County. According to Stephanie, Health Care for the Homeless has benefited from these connections and from being linked to the larger, county system. Here are two examples:
- Health Care for the Homeless has access to Epic, the county’s electronic health record. This helps providers avoid duplication of services.
- Health Care for the Homeless has ties with the pharmacy at Hennepin County Medical Center. For instance, when Health Care for the Homeless Harbor Light Center needs prescriptions for its patients, HCMC Saint Anthony pharmacy will deliver them.
 After receiving a bachelor’s degree in women’s studies and public health, Stephanie Abel (right) went to work at a domestic violence shelter. She later decided to go to nursing school. Stephanie has always believed that the best health care is integrative. She recalls writing a paper to faculty at the University of Minnesota to convince them to allow her to pursue a nursing degree that explored the intersection between social services and health care.
Since its inception in January 2012, Hennepin Health has worked to improve health care for the people it serves.
Hennepin Health uses three kinds of outcomes to track health care improvement. They include patient experience (quality and satisfaction), health care utilization, and health care cost. These three kinds of outcomes align with the “Triple Aim,” a framework that was developed by the Institute for Healthcare Improvement to optimize health care performance.
Each month, Hennepin Health monitors its performance on a growing list of outcomes.
Now that Hennepin Health has more than two years of experience behind it, a clearer story is emerging about how the use of health care is changing among Hennepin Health members. The initial results are encouraging.
Three health care utilization outcome graphs are presented below. The data in these graphs compares Hennepin Health claims data from calendar year 2012 against claims data from January through November of calendar year 2013.
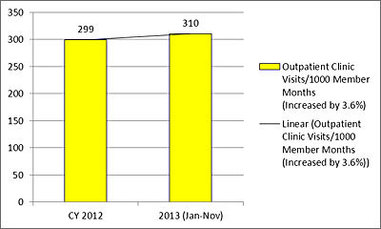 Hennepin Health members have been seeing outpatient clinic providers (including primary care providers) at an increasing rate. This is desirable, since the program hopes that members will use primary care as their main source of care rather than acute care settings. Comparing CY 2012 to January through November of CY 2013, the rate of outpatient visits increased 3.6 percent, suggesting that efforts to engage members with primary care are having an effect.
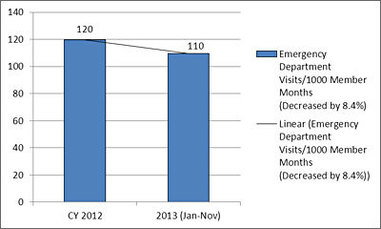 One of the biggest changes in utilization seen among Hennepin Health is the rate of emergency department use, which Hennepin Health hopes to decrease as members seek care in more appropriate settings. Comparing CY 2012 to January through November of CY 2013, the rate of ED visits per 1,000 Hennepin Health members was reduced by 8.4 percent.
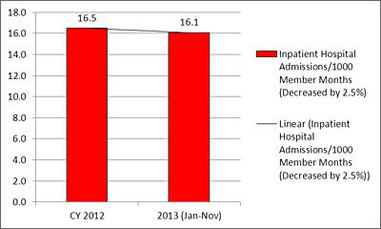 The rate of inpatient admissions from claims data has held relatively flat and remains an area of focus for Hennepin Health, particularly in the area of readmissions. Comparing CY 2012 to January through November of CY 2013, the rate of inpatient hospital admissions decreased by 2.5 percent.
 Hennepin Health just launched a Facebook page. Like our monthly newsletter, the Facebook page is part of Hennepin Health’s strategy to improve internal and external communication. Postings will include member success stories, spotlights on providers and projects, protocol and policy changes, and information about upcoming events.
Please “like” Hennepin Health at: www.facebook.com/hennepinhealthcare
Do you know someone who joined Hennepin Health between January 1 and March 1, 2014?
Hennepin Health is holding a new member event on Wednesday, March 26, from 1 to 3:30 pm. at the Grain Exchange Building in downtown Minneapolis (Suite 780, 301 4th Avenue South).
Members will meet Hennepin Health care coordinators and learn more about the benefit set.
If a member needs transportation to the event, they should call Metropolitan Health Plan’s Member Services at:
1-800-647-0550 (toll-free) or 1-800-627-3529 (TTY)
8 to 4:30 p.m., Monday – Friday

By: Clinton with Tom Davis, Intensive Case Management Team vocational counselor
Clinton was referred to Hennepin Health’s Intensive Case Management Team (ICMT) in 2013 when he was hospitalized for a suicide attempt. (It was his fourth hospitalization that year.) At the time, he had also been participating in treatment for methamphetamine addiction. He was “mentally and physically in very poor health and didn’t care about anything.”
While still in the hospital, he met with ToiJya Holyfield a social worker with the ICMT. She arranged for him to begin treatment at the Professional Counseling Center (PCC) in Delano, Minnesota. Tom Haselman, ICMT supervisor, provided Clinton with a ride to the PCC. During the ride, Clinton had some hesitation about entering treatment. However, with encouragement from Tom, he decided to follow through.
Clinton now says that the PCC was “an amazing program that took time with me, which was just what I needed.” He received both chemical health and mental health treatment at the PCC and continues to be engaged in their program.
Shortly after beginning treatment, Clinton was referred to Tom Davis, one of the ICMT vocational counselors.
Clinton related a work history in the hospitality industry. He said he would like to return to that work but believed that one “sticking point” was his lack of a college degree. He wanted to get the credentials that would go along with his work history, thinking that the combination would allow him to advance in the field.
Tom provided him with information about the Alliss grant, helped him complete his application for student financial aid, and provided him with information about registering for a class at Saint Paul College. Clinton enrolled in an intermediate algebra course to get accustomed to college and to complete some of his prerequisites.
Recently, members of the ICMT (Jodi Smith, case management assistant; Lindsay Erickson, chemical health counselor; and Tom Davis, vocational counselor) had a care conference with Clinton and his counselor at the PCC. Clinton is maintaining his sobriety, engaging in therapy, living in sober housing, participating in aftercare and health realization meetings, and attending school.
Clinton is appreciative of the support of the ICMT and Hennepin Health. He particularly notes that Hennepin Health’s coverage for dentures has been “life changing.” According to Clinton, the “collaboration of Hennepin County (ICMT) and Hennepin Health has helped guide me and gave me access to things I need to get my life in order. The team showed a great deal of care and compassion. I have had time to look, reset, and realize my value.”
|